How to Credential Psychiatry Providers in 2026

The year 2026 marks a pivotal era for mental health services. As the demand for psychiatric care continues to surge, the behavioral health enrollment landscape has become increasingly complex, demanding a high level of precision from administrative leaders. For The Veracity Group, ensuring that your psychiatry providers are fully enrolled and ready to bill is the backbone of professional credibility and financial sustainability. In this environment, a single missing document or an outdated attestation can halt your revenue cycle for months. You must treat the enrollment process as a high-stakes strategic initiative rather than a back-office chore. This guide provides the definitive roadmap for navigating behavioral health provider enrollment in 2026, ensuring your physiatrists and psychiatrists are cleared to provide life-saving care without administrative delay. The Evolving Behavioral Health Enrollment Landscape The shift toward integrated care models and the expansion of telehealth have fundamentally altered how payers view psychiatry. In 2026, payers are no longer just looking for a medical license; they are scrutinizing provider networks for quality metrics, specialized certifications, and multi-state compliance. The behavioral health enrollment landscape is now characterized by stricter “primary source verification” (PSV) standards. Payers are utilizing advanced AI-driven systems to cross-reference NPI data, DEA registrations, and state board actions in real-time. This means any discrepancy in your provider’s file is flagged instantly, leading to immediate application rejection. To maintain a competitive edge, your practice must adopt a “zero-defect” mentality when submitting enrollment packets. Essential Documentation for 2026 Psychiatry Enrollment To begin the behavioral health provider enrollment journey, you must compile a comprehensive digital dossier. The standard for “complete” has been raised, and you will need to provide more than just a CV. 1. Medical Licensure and Board Certification Every psychiatrist must hold a current, unrestricted medical license (MD or DO) in the state where they practice: and increasingly, in every state where their patients reside if they utilize telehealth. Furthermore, most high-tier commercial insurance panels now mandate board certification through the American Board of Psychiatry and Neurology (ABPN). Without active ABPN status, your providers may be excluded from “Gold Card” or preferred provider tiers that offer higher reimbursement rates. 2. DEA Registration and the MATE Act For psychiatrists, a valid DEA registration (Schedules II-V) is non-negotiable. In 2026, payers also verify compliance with the MATE Act, ensuring providers have completed the required training on treating and managing patients with opioid or other substance use disorders. Ensure that your provider’s DEA address matches their primary practice location to avoid “location mismatch” denials. 3. Professional Liability Insurance You must provide a current Certificate of Insurance (COI) that specifically covers psychiatric services. Many payers now require a minimum of $1 million per occurrence and $3 million aggregate in coverage. Ensure the policy is active and the “claims-made” or “occurrence” type is clearly stated. 4. CAQH ProView Accuracy The Council for International Quality Healthcare (CAQH) remains the industry standard, but in 2026, “current” means an attestation within the last 120 days. If a provider’s CAQH profile is even one day out of date, commercial payers like Aetna, Cigna, and UnitedHealthcare will automatically pause the enrollment process. Navigating Medicare and PECOS for Psychiatry Medicare is the largest payer for many psychiatric practices, particularly those serving geriatric populations or specialized clinics. Enrollment in Medicare is handled through the Provider Enrollment, Chain, and Ownership System (PECOS). For psychiatry, the CMS-855I form is the standard for individual practitioners, while the CMS-855B is used for group practices. A common pitfall occurs during the reassignment of benefits. You must ensure that the individual provider’s NPI is correctly linked to the group’s Tax ID. Failure to complete this “linkage” results in claims being processed as “out-of-network,” leading to massive revenue leakage. Furthermore, Medicare has expanded its coverage for Collaborative Care Models (CoCM). When enrolling, ensure your practice is registered to bill codes like G0502, G0503, and G0504. For more insights on why these processes can be so intricate, see our deep dive on why behavioral health provider enrollment is so hard. Telehealth and Multi-State Enrollment Challenges In 2026, psychiatry is no longer bound by physical office walls. However, the behavioral health enrollment landscape for telehealth is a patchwork of state regulations. If your provider is seeing patients across state lines, you must manage multi-state Medicaid provider enrollment and commercial credentialing for each specific jurisdiction. This is a high-risk area for compliance. Many practices mistakenly believe that a single state license is sufficient for telehealth. This is a dangerous assumption. Each state’s Board of Medicine and each payer has unique requirements. To master this complexity, refer to our guide on mastering multi-state Medicaid provider enrollment to ensure your virtual clinic remains compliant and billable. Integrating Multidisciplinary Mental Health Teams Modern psychiatry practices often include a mix of MDs, DOs, psychologists, and addiction specialists. Your enrollment strategy must account for these different provider types simultaneously. As you expand your mental health services, you may find that enrolling psychology providers follows a similar but distinct documentation path, focusing more on doctoral degrees and clinical internships rather than DEA registrations. Similarly, for practices specializing in dual diagnosis, understanding the nuances of addiction medicine provider enrollment is the next logical step in your growth strategy. The American Psychiatric Association (APA) emphasizes the importance of these multidisciplinary teams, but from an enrollment perspective, they double the administrative burden. Each provider type has different “effective dates” and “enrollment windows,” meaning you must track dozens of parallel timelines to prevent gaps in coverage. The High Cost of Enrollment Delays In 2026, the timeline for commercial payer enrollment typically spans 90 to 150 days. If you wait until a provider starts their first day to begin the application, you are looking at nearly half a year of lost revenue. Consider a psychiatrist who sees 15 patients a day with an average reimbursement of $200 per visit. A 120-day enrollment delay represents a $360,000 loss in gross revenue. This is not a hypothetical scenario; it is a mathematical certainty for practices that do not
How to Credential Physical Therapy Providers in 2026

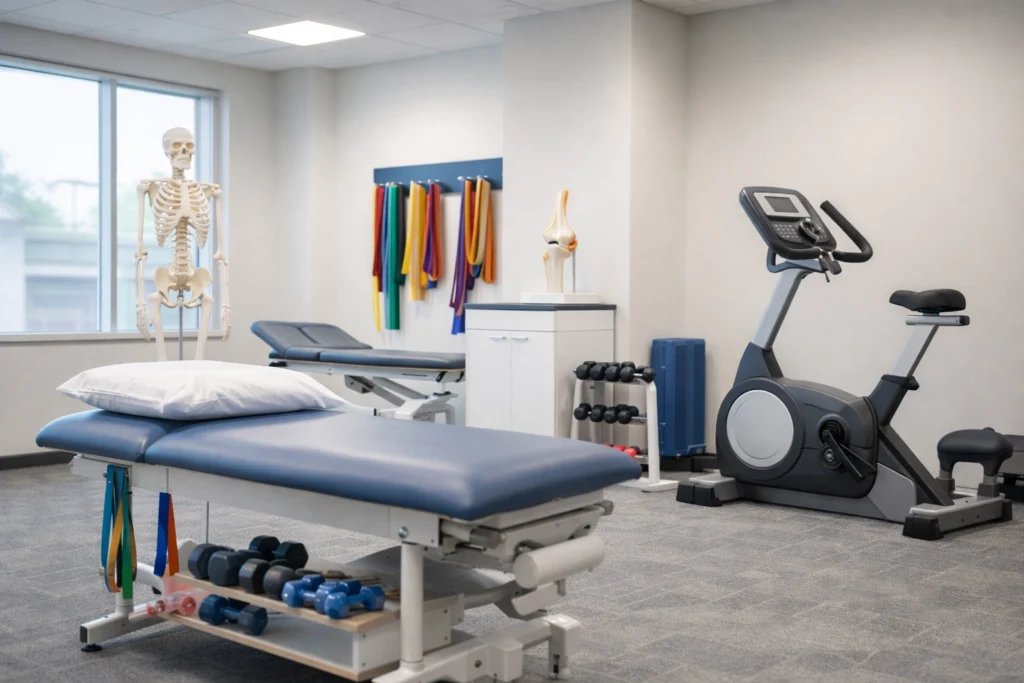
In the rapidly evolving landscape of 2026, Physical Therapy enrollment 2026 is no longer a back-office administrative task; it is a critical strategic driver for any successful rehabilitation practice. As the demand for non-invasive musculoskeletal care surges, the speed and accuracy of your medical provider enrollment services will directly determine your facility’s financial health. A single missed checkbox or an outdated license scan will result in months of “pending” status, leaving your providers unable to treat patients or, worse, treating them without the ability to bill. The Veracity Group understands that for Physical Therapists (PTs) and Physical Therapist Assistants (PTAs), the process is uniquely rigorous. You are navigating a world of PT Compact privileges, Doctorate of Physical Therapy (DPT) verification, and stringent Medicare site inspections. To maintain a competitive edge, you must treat the enrollment process with the same precision you apply to a patient’s plan of care. The High Cost of Enrollment Delays in 2026 The year 2026 has introduced heightened scrutiny from commercial payers and government agencies alike. Insurance carriers are no longer granting “grace periods” for providers waiting on participation status. If a provider is not fully loaded into the payer’s system, claims for common procedures: such as therapeutic exercise (CPT 97110) or manual therapy (CPT 97140): will be denied immediately. For a high-volume PT clinic, a 90-day delay in enrollment for a single provider can represent over $60,000 in unrealized revenue. This is the silent driver of practice failure. You must stay ahead of the curve by initiating the process at least four months before a provider’s start date. Alt Tag: Watercolor illustration of a modern physical therapy rehabilitation center interior representing professional enrollment standards. Essential Documentation for PT Providers Before you even log into a portal, you must gather a comprehensive “passport to success.” In 2026, payers are utilizing AI-driven scraping tools to verify these documents against national databases. Any discrepancy will trigger a manual review, adding weeks to your timeline. The Mandatory PT Checklist Includes: Current State Licensure: Must be valid with an expiration date at least six months in the future. PT Compact Privileges: If practicing across state lines, you must provide the specific privilege authorization from the Federation of State Boards of Physical Therapy (FSBPT). DPT Degree Verification: Official transcripts or primary source verification of the Doctorate of Physical Therapy. NPI Type 1 and Type 2: Individual NPIs are mandatory, but if you are a group practice, your Type 2 NPI must be correctly linked in the NPPES registry. Professional Liability Insurance: Coverage must meet the 2026 minimums, typically $1 million per occurrence and $3 million aggregate. CAQH ProView Profile: This must be 100% complete and attested within the last 45 days. The Step-by-Step PT Enrollment Roadmap Successfully navigating the maze of medical provider enrollment services requires a disciplined, sequential approach. Skipping a step or performing them out of order is a recipe for administrative gridlock. 1. The CAQH Foundation Your CAQH profile is the backbone of professional credibility. Ensure every work history gap of more than 30 days is explained. In 2026, payers are specifically looking for “continuity of clinical excellence.” Upload your current W-9 and ensure the “Practice Location” address matches the USPS standardized format exactly. 2. Medicare PECOS Submission For PTs, Medicare enrollment is often the most grueling phase. Unlike some other specialties, PT practices are subject to high-risk screening. You must submit your 855I (for individuals) or 855B (for groups) via the PECOS portal. Ensure you are prepared for a Medicare Site Visit, where inspectors will verify your gym equipment, ADA compliance, and operational readiness. 3. Commercial Payer Strategy Do not wait for Medicare approval to start commercial applications. Identify the top 10 payers in your region and submit applications concurrently. While the American Physical Therapy Association (APTA) provides excellent clinical resources, the administrative burden of tracking 10 different payer portals falls on your practice. You must log weekly follow-ups and record every interaction ID. Alt Tag: Watercolor illustration of a healthcare workspace for organized physical therapy enrollment documentation and payer follow-ups. 2026 Regulatory Changes You Must Know The regulatory environment in 2026 has shifted toward digital-first verification. If your practice is still relying on paper-based workflows, you are already behind. Digital Verification and State Board APIs Most major payers now use real-time APIs to pull data directly from state licensing boards. This means if your address is updated at the state level but not in CAQH, the system will flag a mismatch. Consistency across all platforms: NPPES, CAQH, and State Boards: is mandatory. Enhanced Medicare Screening Effective January 1, 2026, CMS implemented enhanced background checks for Physical Therapy providers in certain “high-utilization” geographic areas. This may include fingerprinting requirements that were previously reserved for only high-risk DME (Durable Medical Equipment) suppliers. If your PT practice also provides orthotics or specialized bracing, you face double the scrutiny. This complexity is similar to what we see in specialized surgical settings; for instance, navigating medical group enrollment for surgery centers requires a similar level of attention to facility-specific compliance. Addressing the Behavioral Health Integration Many PT practices in 2026 are integrating holistic wellness and pain management counseling. If your practice includes these services, be aware that the enrollment hurdles for those providers are even more specialized. You can learn more about why behavioral health provider enrollment is so hard to ensure your integrated team is fully covered. Alt Tag: Watercolor illustration of a goniometer and clinic tools representing the physical therapy enrollment lifecycle and specialty nuances. Specialized PT Enrollment Nuances Physical Therapy is not a “one-size-fits-all” specialty. To ensure full reimbursement, your enrollment must reflect your specific scope of practice. Durable Medical Equipment (DME): If you dispense TENS units, braces, or custom orthotics, you must have a separate DMEPOS enrollment. This requires a separate bond and a specific site inspection. PT Compact (FSBPT): For practices near state borders, leveraging the FSBPT Compact is a game-changer. However, you must enroll in the specific state’s Medicaid program separately, even if you
How to Credential Pediatric Providers in 2026

In 2026, the landscape for pediatric provider enrollment is defined by one word: precision. Payers have moved away from broad data aggregators and toward rigorous, primary-source verification. For your pediatric practice, this means the days of “submit and wait” are over. Today, a single missing vaccination record or an outdated developmental screening certification can stall your revenue cycle for months. The Veracity Group understands that pediatric enrollment is the backbone of your professional credibility. Whether you are onboarding a new associate or expanding into a multi-state telehealth model, your enrollment strategy must be proactive, detailed, and aligned with the latest federal mandates. The 2026 Pediatric Enrollment Standards The bar for entry has been raised. As of January 1, 2026, CMS and private payers have implemented enhanced verification standards that require direct confirmation from medical schools, residency programs, and state licensing boards. Reliance on third-party databases is no longer acceptable; payers now demand “source-of-truth” documentation for every line item on an application. For pediatricians, this process is even more granular. You must demonstrate compliance with Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) regulations, which are central to state Medicaid and CHIP panels. Failure to provide primary-source proof of pediatric-specific qualifications will result in immediate application rejection. Image Alt Tag: A professional, high-end contemporary pediatric clinic waiting area with clean lines and soft lighting, representing a modern healthcare environment. Essential Documentation for Pediatric Onboarding To avoid the high cost of delays, your practice must have a “gold standard” digital credentialing folder ready before you even begin the CAQH or PECOS process. In 2026, the following documents are non-negotiable: Primary Source Education Verification: Original medical degrees and official transcripts sent directly from the institution. Pediatric Board Certifications: Current certificates with active verification codes from the American Board of Pediatrics. Comprehensive Malpractice History: A full 10-year history of coverage declarations, including any claims history or gap explanations. Vaccination and Health Records: Proof of immunizations meeting the latest CDC guidelines for healthcare providers. DEA and State Licenses: Certified copies for every state where the provider will treat patients, especially crucial for those navigating multi-state Medicaid provider enrollment. Navigating Medicaid and CHIP in 2026 Because a significant portion of pediatric care is funded through Medicaid and the Children’s Health Insurance Program (CHIP), your enrollment in these programs is the lifeblood of your practice. In 2026, state agencies have shortened the revalidation cycle for pediatric specialties from five years down to three. EPSDT compliance is a major focus this year. Payers are auditing pediatric providers to ensure they possess the specific credentials required to perform developmental screenings and lead-level testing. If your provider’s enrollment file does not explicitly list these qualifications, you may find your claims for these services denied, even if the provider is “enrolled” in the general network. Image Alt Tag: An abstract geometric professional design representing the structured and interconnected nature of healthcare provider data and enrollment workflows. CMS Enrollment and the PECOS Update The Centers for Medicare & Medicaid Services (CMS) has introduced significant changes to the PECOS system for 2026. The enrollment application fee for institutional providers has been adjusted to $750, and there is a renewed focus on fingerprint-based background checks for providers categorized as high-risk. When submitting the CMS-855I or CMS-855B forms, the National Provider Identifier (NPI) must match your NPPES data with 100% accuracy. Discrepancies in addresses or legal names between these systems are the leading cause of enrollment holds in 2026. If you find the federal system overwhelming, our guide on navigating the maze of CAQH and Medicare enrollment provides a roadmap to avoid common pitfalls. Telehealth and the Interstate Compact Pediatric telehealth has expanded rapidly, and the Interstate Medical Licensure Compact (IMLC) now includes 40 states. However, while the IMLC streamlines the licensing process, it does not bypass the enrollment process. Each state where a patient is located requires a separate enrollment into that state’s Medicaid program and relevant private payer panels. In 2026, states like New York and California have added telehealth-specific credentialing requirements. You must provide proof of specialized training or platform security compliance to be authorized for virtual pediatric visits. This is the “silent driver” of revenue growth: or revenue loss: for modern pediatric groups. The Impact of Quality Metrics on Enrollment Your reputation now precedes your enrollment. In 2026, Value-Based Care (VBC) metrics and MIPS scores are integrated into the credentialing review process for Medicare Advantage and major commercial payers. Payers are actively reviewing: Patient Experience Scores: High-performing practices are fast-tracked, while those with poor satisfaction data face extended “quality reviews.” Outcome Metrics: For pediatrics, this includes childhood immunization status (CIS) and well-child visit frequency. Professionalism: Some payers have even implemented quarterly social media and public record reviews to identify concerns before they become liabilities. Ensuring your data is accurately reflected in your CAQH profile is essential to demonstrating your practice’s commitment to quality. Image Alt Tag: A minimalist professional medical office desk with a tablet showing a secure data dashboard, reflecting modern provider data management. Why Outsourcing is the 2026 Solution The complexity of pediatric provider enrollment in 2026 makes internal management a high-risk endeavor. The Veracity Group offers specialized services that handle the heavy lifting of Medicaid/CHIP applications and state-specific pediatric regulations. Our technology-based tracking and expert oversight can reduce your denial risk by 20-30%. When you partner with us, you aren’t just filing paperwork; you are securing your practice’s financial future. From contracting to demographic updates, we ensure that your providers are ready to see patients and get paid without the 120-day wait times typical of unmanaged applications. Summary of Best Practices To succeed in 2026, your pediatric practice must adopt these habits: Audit your NPPES and CAQH profiles monthly. Ensure all addresses and contact information are current. Monitor the OIG exclusion list. Perform monthly checks against state Medicaid exclusion lists and the System for Award Management (SAM) database. Stay ahead of NCQA timelines. The new 90-day window for certified organizations means you have less time to respond
How to Credential Pain Management Providers in 2026

The landscape of pain management is undergoing a seismic shift in 2026. As the healthcare industry intensifies its focus on the opioid crisis and patient safety, the process for how to credential pain management providers has evolved from a routine administrative task into a high-stakes compliance gauntlet. For practice managers and owners, understanding these changes is the difference between a thriving revenue cycle and a series of devastating claim denials. Pain management is now classified by most major payers as a high-risk specialty. This designation carries heavy implications for your enrollment timelines and documentation accuracy. To maintain your practice’s financial health, you must treat enrollment not as a periodic checkbox, but as a continuous state of readiness. The 2026 “High-Risk” Designation and Accelerated Cycles In years past, a pain management provider could expect a standard three-year recredentialing cycle. In 2026, those days are over. Most commercial payers and Medicare Advantage plans have shifted to accelerated recredentialing cycles of 18 to 24 months. This heightened scrutiny is driven by the need for real-time oversight of prescribing patterns and interventional procedures. If your administrative team is still waiting for a three-year “tickler” alarm to go off, you will miss critical deadlines. Missing a recredentialing window in this specialty results in immediate de-activation, leading to a complete cessation of reimbursements for high-revenue procedures like epidural steroid injections (CPT 62323) or spinal cord stimulator trials (CPT 63650). Alt Text: A professional glass-walled medical office where administrators are managing digital provider enrollment files for a pain management clinic. Enhanced Background Screening: Beyond the Initial Hire The most significant change in 2026 is the requirement for continuous monitoring. Payers now expect practices to conduct monthly OIG exclusion list screenings. This involves checking every provider and clinical staff member against federal and state Medicaid exclusion databases, as well as the System for Award Management (SAM). It is no longer sufficient to verify a provider’s standing at the time of hire. A single “hit” on an exclusion list that remains unaddressed for thirty days will trigger a full audit and potential clawback of all funds paid during the period of non-compliance. Furthermore, some forward-leaning payers have integrated quarterly social media and public sentiment reviews into their enrollment criteria to identify potential professionalism concerns or unethical marketing of controlled substances before they become a liability. The 2026 Documentation Arsenal When you begin the process of how to credential pain management providers, your documentation must be flawless. Any gap in history or missing verification code will result in the application being returned, potentially adding 60 to 90 days to your enrollment timeline. To succeed in 2026, you must compile a comprehensive digital dossier that includes: Original Medical Degree and Official Transcripts: Digitized, certified copies sent directly from the institution when required. Multi-State Licenses: As telemedicine and multi-site clinics expand, you must hold active, unencumbered licenses for every state where the patient resides at the time of service. Current DEA Certificate: This must reflect the correct practice address and include all relevant schedules (II-V). 10-Year Malpractice History: You must provide insurance declarations showing a continuous decade of coverage. Any “tail” coverage or gap must be explained with a signed, dated letter of explanation. Board Certification Verification: Direct verification from the American Board of Anesthesiology or other relevant specialty boards is mandatory. For practices managing multiple locations or providers transitioning from hospital settings, managing these documents is the backbone of professional credibility. If you are navigating this for the first time, our guide on navigating the maze of CAQH and Medicare enrollment provides the strategic framework needed to organize these assets effectively. Quality Metrics and MIPS: The New Enrollment Gatekeepers In 2026, clinical skill is only half of the equation. Enrollment is now inextricably linked to quality metric performance. Medicare and a growing number of private payers now require MIPS (Merit-based Incentive Payment System) scores to be submitted or accessible during the initial credentialing phase. Providers with scores falling below the national threshold face significant barriers to entry. Payers are looking for data on: Opioid use disorder screening rates. Patient satisfaction scores (HCAHPS). Functional status improvement following interventional procedures. If a provider has a history of poor patient satisfaction or low MIPS performance, a payer may deny their “network adequacy” request, effectively locking them out of the panel regardless of their board certifications. This makes the demographic updates and quality reporting and tracking within your CAQH profile more critical than ever. Alt Text: A detailed digital dashboard showing MIPS quality scores and patient satisfaction metrics used for provider enrollment in 2026. Board Certification Pathways for Pain Management Payer enrollment departments in 2026 are stricter regarding which board certifications qualify a provider for the “Pain Management” specialty designation. To be credentialed as a specialist rather than a generalist, the provider must follow one of these verified pathways recognized by the Centers for Medicare & Medicaid Services (CMS): Subspecialty Certification: A formal Pain Management subspecialty conferred by the American Board of Anesthesiology, Emergency Medicine, Family Medicine, Psychiatry and Neurology, or Physical Medicine and Rehabilitation. The 50% Rule: Documentation proving the provider has spent at least 50% of their practice time in pain management for the previous two years. Post-Graduate Training: Completion of at least 12 months of specialized post-graduate fellowship training in an ACGME-accredited pain management program. Failure to prove one of these pathways will result in the provider being “downgraded” in the payer directory. This not only affects your reimbursement rates but also limits the provider’s visibility to patients searching specifically for pain specialists. Addressing the “Silent Driver” of Denials: Work History Gaps A common pitfall in the 2026 enrollment process is the failure to account for work history gaps. Payers now utilize automated systems to flag any period exceeding 30 days where a provider was not actively employed or in a training program. You must provide a month-year to month-year timeline for the provider’s entire professional life post-medical school. If a provider took a sabbatical or a leave of absence, you
How to Credential Orthopedic Providers in 2026
In the high-stakes landscape of 2026 healthcare, orthopedic practices face a rigorous regulatory environment where administrative precision is as vital as surgical accuracy. For an orthopedic surgeon, the ability to perform a complex total joint arthroplasty or a delicate spinal fusion is moot if the provider is not properly enrolled with the necessary payers. The Veracity Group understands that in orthopedics, any delay in the enrollment process translates directly into thousands of dollars in lost revenue and a bottleneck in patient access to specialized care. To maintain a healthy revenue cycle, your practice must navigate a labyrinth of primary source verification, compressed timelines, and specialty-specific requirements. This guide outlines the essential steps and strategic maneuvers required to successfully manage orthopedic provider enrollment in 2026. The Critical Documentation Foundation The backbone of a successful enrollment application is the underlying documentation. In 2026, payers have moved beyond simple data entry; they require a comprehensive digital dossier that proves a provider’s qualifications and standing. For orthopedic specialists, this includes several high-level requirements that go beyond general medicine. 1. Board Certification and Education Payers strictly verify certification through the American Board of Orthopaedic Surgery (ABOS) or the American Osteopathic Board of Orthopedic Surgery. In 2026, the absence of an "active" status or a failure to demonstrate ongoing Maintenance of Certification (MOC) will result in an immediate application rejection. Ensure that all fellowship certificates: whether in sports medicine, hand surgery, or pediatric orthopedics: are included to satisfy sub-specialty enrollment requirements. 2. Surgical Privileges and Admitting Arrangements Unlike primary care providers, orthopedic surgeons are defined by their ability to operate. Commercial payers and Medicare now require documented proof of active surgical privileges at a minimum of one Joint Commission-accredited hospital or Ambulatory Surgery Center (ASC). If your provider is joining a group but does not yet have local hospital privileges, you must establish formal admitting arrangements to satisfy payer requirements. Failure to align these privileges with the enrollment timeline will halt the process entirely. 3. Professional Liability Insurance Orthopedics remains a high-risk specialty. Payers in 2026 require malpractice face sheets that explicitly list the provider’s name, the specialty of "Orthopedic Surgery," and coverage limits that meet or exceed state-mandated minimums. If your practice operates across state lines, the policy must reflect coverage for every jurisdiction where the provider sees patients. Style: A clean, modern architectural view of a high-tech orthopedic surgical suite, emphasizing precision and professional structure. Navigating the 2026 Timeline: Speed is a Requirement The industry has shifted. As of 2026, accredited organizations have seen their credentialing and enrollment windows compressed significantly. What used to take six months must now be completed in 90 to 120 days. This shift is driven by the National Committee for Quality Assurance (NCQA) and a collective push for faster patient access to care. For your orthopedic practice, this means there is zero margin for error. A single typo in a National Provider Identifier (NPI) record or an outdated address on a CAQH profile will trigger a "return to sender" status. In the orthopedic world, where specialized equipment and surgical blocks are scheduled months in advance, a 30-day delay in enrollment can disrupt an entire surgical calendar. Managing these tight windows requires a proactive approach. You must initiate the process the moment a contract is signed, rather than waiting for the provider’s start date. If you are managing a larger facility, understanding medical group enrollment for surgery centers is essential to avoid common compliance pitfalls that often ensnare orthopedic groups. The Role of CAQH ProView and Real-Time Verification In 2026, the CAQH ProView profile serves as the "digital passport" for orthopedic providers. It is no longer a "set it and forget it" platform. Payers now use automated API integrations to pull data from CAQH weekly. If the data in CAQH does not perfectly match the data on the provider’s state license or NPI record, the automated systems will flag the provider for manual review, adding weeks to the timeline. Key areas to maintain in CAQH for orthopedic surgeons include: Gap-Free Work History: Any gap over 30 days must be explained. This includes time taken for fellowship transitions or relocations. Malpractice Claims History: Orthopedic surgeons must provide detailed explanations for any historical claims, even if they were dismissed. Disclosure Questions: These must be answered with 100% honesty. 2026 verification tools are linked to federal databases that identify any previous sanctions or disciplinary actions instantly. Ensuring your CAQH profile is optimized is a core component of navigating the maze of Medicare enrollment, a process that remains the gold standard for all other commercial payers. DMEPOS and Specialty-Specific Enrollment One of the most overlooked aspects of orthopedic enrollment is the DMEPOS (Durable Medical Equipment, Prosthetics, Orthotics, and Supplies) requirement. Most orthopedic practices dispense braces, boots, or crutches directly to patients. To bill for these items, the practice and the individual providers must be enrolled as DMEPOS suppliers. This requires a separate application through the National Supplier Clearinghouse (NSC) using the CMS-855S form. In 2026, the site visit requirements for DMEPOS enrollment are stricter than ever. Your facility must be prepared for a physical inspection to ensure compliance with specialized storage and patient access standards. If your orthopedic providers are not correctly enrolled as DMEPOS suppliers, you will face automatic denials for all Level II HCPCS codes (such as L1845 for knee braces), resulting in significant unrecovered overhead costs. Style: An infographic-style, clean line illustration showing the flow of orthopedic provider data from licensing boards to payer systems. Continuous Monitoring: Beyond Initial Enrollment In 2026, the concept of "re-credentialing every three years" is largely obsolete. The industry has moved toward continuous monitoring. Payers now subscribe to databases that alert them within 24 hours if an orthopedic surgeon’s license is flagged, if their DEA registration expires, or if they are added to the OIG exclusion list. Veracity recommends a 30-day internal audit cycle for all orthopedic providers. You must monitor: State Medical Licenses: Orthopedic surgeons often hold multiple licenses for cross-state surgical consultations. DEA
How to Credential Oncology Providers in 2026
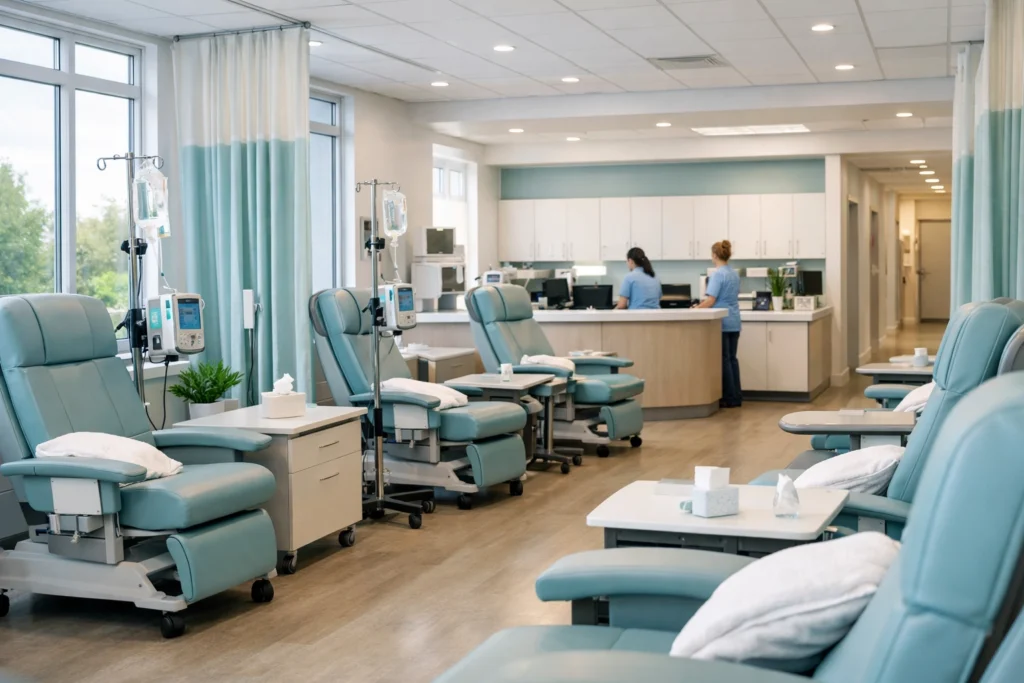
In the high-stakes world of oncology, delays in provider enrollment do more than just stall your revenue cycle; they directly impact the delivery of life-saving treatments to vulnerable patient populations. As we move through 2026, the regulatory landscape for oncology provider enrollment has become more rigorous, requiring a level of precision that leaves zero room for error. Whether you are onboarding a medical oncologist, a radiation oncologist, or a surgical specialist, your practice must adhere to the most current verification standards to ensure uninterrupted participation in payer networks. The complexity of oncology: involving expensive chemotherapy agents, high-tech radiation equipment, and multi-disciplinary care teams: makes these providers a focus of intense scrutiny for insurance carriers. At The Veracity Group, we see firsthand how a single missing document or an outdated CAQH profile can trigger a cascade of claim denials that threaten the financial health of a cancer center. The Foundation of Oncology Enrollment: Core Documentation Credentialing oncology providers in 2026 is a marathon of documentation. You must gather a comprehensive dossier before you even consider submitting an application to a payer. In the current environment, “close enough” is no longer acceptable. Payers are rejecting applications that lack primary source verification or contain even minor discrepancies in work history. To begin, your practice must secure: Original Medical Degrees and Official Transcripts: Digital copies must be high-resolution and certified. State Medical Licenses: You must provide active licenses for every state where the oncologist will practice, including those used for telemedicine consultations. Board Certifications: This is the backbone of professional credibility. For medical oncologists, this means verification through the American Board of Internal Medicine (ABIM). For radiation oncologists, the American Board of Radiology (ABR) is the standard. DEA Certificates: Given the necessity of palliative care and pain management in oncology, a valid DEA certificate with current expiration dates is non-negotiable. Malpractice History: You are required to provide at least 10 years of claims history. Any “gaps” in coverage or practice must be explained with signed, dated statements. Image Description: A high-end, modern oncology consultation room featuring clean architectural lines, minimalist furniture, and a large window overlooking a city. The style is architectural photography, focusing on precision and professionalism. Primary Source Verification: The 2026 Standard Gone are the days when insurance companies relied solely on third-party aggregators to verify a provider’s background. In 2026, Primary Source Verification (PSV) is the only accepted method. This means payers will contact the issuing institutions directly: medical schools, residency programs, and previous employers: to confirm the legitimacy of every claim on a provider’s CV. If your oncology provider completed a fellowship at a specialized institution like Memorial Sloan Kettering Cancer Center, the payer will verify that training directly with the facility. Any lag in response from these institutions will delay your enrollment timeline. This is why proactive outreach is essential. You must ensure that your providers have “cleared the path” by notifying their former programs that verification requests are forthcoming. Navigating CAQH and the Medicare Maze For any oncology practice, Medicare is often the largest payer. Navigating the PECOS (Provider Enrollment, Chain, and Ownership System) is a specialized skill set. Errors in the CMS-855I or CMS-855R forms will result in a “returned” application, forcing you to restart the 90-to-120-day clock. Simultaneously, you must master the CAQH ProView system. This platform acts as the central repository for provider data used by nearly all private payers. In 2026, a “stale” CAQH profile is the leading cause of enrollment delays. You must treat CAQH as a living document, updating it immediately whenever a license is renewed or an address changes. For a deeper look at managing these systems, see our guide on navigating the maze of CAQH and Medicare enrollment. Image Description: A close-up, minimalist shot of a high-tech medical tablet displaying a clean, organized dashboard of provider credentials. The lighting is soft and corporate, emphasizing data clarity and modern healthcare technology. Specialty-Specific Hurdles in Oncology Oncology enrollment carries unique requirements that other specialties might not encounter. Because oncologists frequently work across multiple settings: including outpatient clinics, infusion centers, and hospitals: maintaining hospital privileges is critical. Most payers will not complete the enrollment of a surgical oncologist without proof of active, unrestricted privileges at an accredited hospital. Furthermore, if your practice operates across state lines: a common occurrence for regional cancer centers: you must stay ahead of varying state mandates. Each state has unique Medicaid requirements and licensing timelines. Our experts at The Veracity Group specialize in mastering multi-state Medicaid provider enrollment to help oncology groups expand their footprint without the administrative headache. Enhanced Screening and Ongoing Monitoring In 2026, credentialing is no longer a “one-and-done” event every three years. It is an ongoing cycle of compliance. Monthly sanctions screenings are now the industry standard. You must monitor: OIG Exclusion List: Ensuring no provider is barred from federal programs. SAM (System for Award Management): Verifying eligibility for government contracts. State Medicaid Exclusion Lists: Crucial for multi-state practices. Failure to identify a sanctioned provider on your team can lead to massive fines and the recoupment of all payments made to that provider. Veracity recommends implementing a system for continuous demographic updates to ensure your practice information remains accurate in all payer directories. The Financial Consequence of Delay The cost of a credentialing error in oncology is astronomical. Consider a medical oncologist who is unable to bill for chemotherapy administration for 90 days due to an enrollment delay. The lost revenue from drug costs alone can reach hundreds of thousands of dollars, not to mention the professional fees. This “silent driver” of lost profit is why high-growth practices outsource these functions. Payers have also shortened their “grace periods.” In the past, some insurers allowed a 60-day window to finalize enrollment while still paying claims. In 2026, most major payers, including UnitedHealthcare and Aetna, have moved toward a strict “no enrollment, no payment” policy. If your provider is not fully loaded in their system, your claims will be denied, and they are often non-rebillable.
How to Credential OB/GYN Providers in 2026
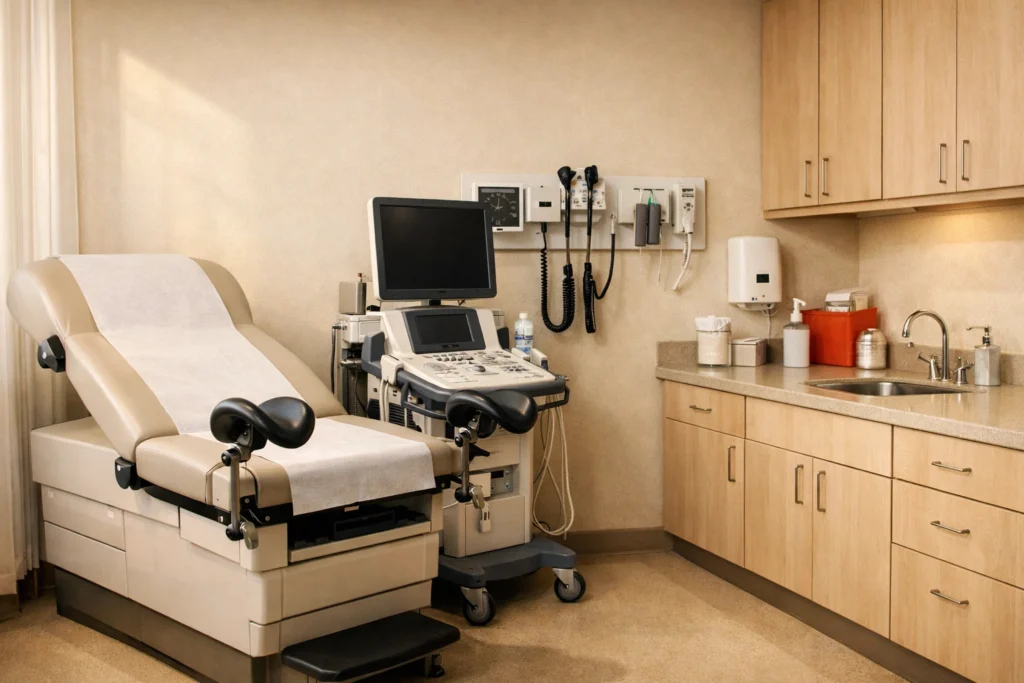
In the rapidly evolving healthcare landscape of 2026, the administrative burden of bringing a new OB/GYN into your practice has reached a critical peak. For specialized fields that bridge the gap between primary care and major surgery, the margin for error in provider enrollment is non-existent. How to credential OB/GYN providers in 2026 is no longer a question of simple paperwork; it is a high-stakes race against shifting federal mandates and rigorous specialty board requirements. Delays in the enrollment process do more than stall a provider’s start date: they paralyze your revenue cycle and restrict patient access to essential reproductive health services. As payers implement more aggressive verification technologies, your practice must adopt a proactive, data-driven strategy to ensure your clinicians are fully authorized to bill from day one. The 2026 Regulatory Climate for OB/GYN Enrollment The start of 2026 brought a wave of changes from the Centers for Medicare & Medicaid Services (CMS) that directly impact high-volume specialties. Enhanced fingerprint-based background checks are now a standard requirement for higher-risk categories, and the revalidation cycle for many surgical specialists has been compressed from five years down to three. Furthermore, the shift toward continuous monitoring means that “set it and forget it” credentialing is a thing of the past. Major payers now mandate monthly sanction screenings against the OIG exclusion list and the System for Award Management (SAM) database. For an OB/GYN practice, a single overlooked expiration or a missed state license update can lead to immediate claim denials across your entire patient panel. Essential Documentation for the Modern OB/GYN To navigate the 2026 enrollment maze, your documentation must be exhaustive and digitally accessible. The complexity of OB/GYN care: encompassing office visits, labor and delivery, and gynecological surgery: requires a specific set of credentials that other specialties may overlook. You must secure the following primary source verifications before initiating any payer applications: Board Certification Verification: Evidence of certification through the American Board of Obstetrics and Gynecology (ABOG). In 2026, payers are verifying not just the certificate, but the specific maintenance of certification (MOC) status in real-time. Surgical Skills Certification: Documentation of completion of a Surgical Skills Program, such as FLS (Fundamentals of Laparoscopic Surgery) or EMIGS (Essentials in Minimally Invasive Gynecologic Surgery), is now a standard prerequisite for hospital privileges and many high-tier insurance contracts. Malpractice History: OB/GYN remains a high-liability specialty. You must provide a full 10-year history of malpractice coverage, including detailed “claims-made” or “occurrence” declarations and explanations for any settlements or pending litigation. Work History Clarity: Payers in 2026 are scrutinizing gaps in employment more than ever. Any gap exceeding 30 days must be accompanied by a written explanation. Telehealth Credentials: If your provider offers virtual prenatal check-ups or contraceptive counseling, ensure they hold the specific telehealth endorsements now required by states like New York and California for Medicaid reimbursement. Style: A clean, professional paper cutout illustration of a modern OB/GYN clinical suite, featuring an exam table and ultrasound equipment in soft, layered tones. Navigating the CAQH and Medicare Workflow The CAQH ProView profile remains the backbone of professional credibility in the enrollment world. However, in 2026, the integration between CAQH and individual payer portals has become more complex. An incomplete profile is a “silent driver” of revenue loss; if your CAQH data doesn’t perfectly mirror your NPPES (NPI) registry and your PECOS enrollment, the system will trigger an automatic rejection. When managing how to credential OB/GYN providers in 2026, your workflow should follow this strict sequence: Step 1: Update the NPI Registry. Ensure the taxonomy codes accurately reflect the OB/GYN specialty and any sub-specialties like Maternal-Fetal Medicine (MFM). Step 2: CAQH Attestation. Complete the profile with 2026-compliant immunization records and current DEA certificates. Step 3: Medicare Enrollment (PECOS). Submit the 855I or 855O forms immediately, as Medicare approval is often the prerequisite for private payer secondary enrollment. Step 4: Hospital Privilege Finalization. Since OB/GYNs rely on facility access for deliveries and surgeries, the coordination between the practice and the hospital’s medical staff office is vital. For a deeper look at the technical requirements of these platforms, see our guide on navigating the maze of CAQH and Medicare enrollment. The High Cost of Enrollment Delays In the world of OB/GYN, a provider who is not yet “linked” to a contract is a provider who is working for free. The financial consequences of administrative friction are staggering. If a new physician sees 20 patients a day while waiting for a payer to process an application, the practice can easily lose tens of thousands of dollars in uncollectible revenue in a single month. Moreover, patient trust is at stake. When a patient discovers their long-term OB/GYN is suddenly “out of network” due to an enrollment lapse, they are likely to seek care elsewhere. This is why multi-state practices must be particularly vigilant. Each state has unique mandates, such as California’s real-time primary source verification or the strict documentation timelines in Texas. Mastering multi-state Medicaid provider enrollment is essential for groups expanding across state lines. Strategic Solutions for Your Practice Managing the intricacies of OB/GYN enrollment requires more than just administrative effort; it requires a specialized partnership. At The Veracity Group, we understand that your focus should be on patient care: bringing new lives into the world and maintaining the health of your community: not chasing down payer representatives or deciphering updated CMS manuals. By leveraging an expert enrollment service, you gain: Accelerated Timelines: Reducing the standard 120-day window down to the absolute minimum allowed by the payer. Expert Compliance: Ensuring every surgical certification and board MOC update is correctly reflected in your profiles. Revenue Protection: Preventing the “silent” denials that occur when demographic data is out of sync. The landscape of 2026 demands a higher standard of precision. Don’t let your practice’s growth be hindered by outdated enrollment tactics. Whether you are onboarding a new resident or adding a seasoned surgeon, the time to start the process is now. Secure Your Revenue Cycle Today The complexities of OB/GYN enrollment
How to Credential Neurology Providers in 2026

In the high-stakes landscape of 2026 healthcare, neurology stands as one of the most complex specialties to manage from an administrative perspective. With the rise of specialized stroke centers, complex neuro-oncology departments, and an aging population requiring cognitive care, the speed and accuracy of your provider enrollment process will determine your practice’s financial viability. For neurology practices, enrollment is not merely a box to check; it is the backbone of professional credibility and the primary driver of revenue. If a neurosurgeon or a general neurologist is not properly enrolled with payers, your facility is essentially providing high-cost, specialized care for free. In 2026, the margin for error has vanished. Payers are more stringent, timelines are tighter, and the documentation requirements for neurological sub-specialties are more granular than ever. The Neurology Documentation Arsenal: Beyond the Basics To successfully navigate how to credential neurology providers in 2026, you must move beyond generic checklists. Neurology requires a specific set of primary source verifications that reflect the high level of training these specialists undergo. Missing a single sub-specialty certification or failing to provide updated procedure logs for interventional neurology can result in immediate application rejection. You must gather and verify the following documentation before initiating any enrollment applications: Comprehensive Medical Education Records: This includes not only the medical school diploma and transcripts but also specific internship and residency certificates in neurology. ABPN Certification Status: For 2026, you must provide current American Board of Psychiatry and Neurology (ABPN) certification details. If the provider is board-eligible, you must document the specific timeline for their upcoming examination. Sub-Specialty Certifications: Whether the provider focuses on Clinical Neurophysiology, Epilepsy, Neurocritical Care, or Neuromuscular Medicine, these certifications must be submitted to payers to ensure correct reimbursement for specialized CPT codes. Active, Unrestricted State Licenses: You must maintain a full medical license in every state where the provider sees patients, including states where they provide consults via telehealth. DEA and CSR Registrations: Given the controlled substances often prescribed in neurology (for epilepsy or chronic pain management), active DEA certificates with matching practice addresses are non-negotiable. Detailed Work History: You must provide a 10-year employment history without any gaps. If a gap longer than 30 days exists, a written explanation is required to satisfy 2026 NCQA standards. Malpractice Coverage: Current COIs with limits meeting the specific requirements of neurology (which are often higher due to the high-risk nature of the specialty). Image Description: A 3D isometric clinical illustration showing a modern neurology office suite with organized digital workstations and medical imaging displays, representing an efficient administrative environment. Navigating the 2026 NCQA and Payer Tightropes The regulatory environment in 2026 has shifted significantly. The National Committee for Quality Assurance (NCQA) has updated its standards, requiring even more frequent data refreshes and tighter windows for application processing. For accredited organizations, the credentialing window has been reduced from 180 days to just 120 days. For certified organizations, you are now operating on a 90-day timeline. This reduction in time means that proactive management is your only defense against lapses in coverage. At The Veracity Group, we have seen that practices relying on manual tracking or outdated software are the first to suffer from “enrollment lag”: the period where a provider is seeing patients but the payer has not yet finalized their participation status. Continuous monitoring is now a core requirement. Payers no longer wait for a three-year recredentialing cycle to check for sanctions or license expirations. In 2026, automated systems pull data from the National Practitioner Data Bank (NPDB) and state licensing boards in real-time. If your provider’s data is not perfectly aligned across NPPES, CAQH, and payer databases, your claims will be denied. To understand how these systems interact, your team should review our guide on navigating the maze of CAQH and Medicare enrollment. The Critical Importance of the 2026 ABPN Timeline For neurology providers seeking board certification in 2026, the calendar is your master. The ABPN has set strict deadlines for the 2026 examination cycles. For instance, the application deadline for the September 2026 exam is April 6, 2026, with a final late deadline of May 4, 2026. If you are onboarding a new neurologist who is transitioning from a training license to a full license, they must update their information to reflect an active, unrestricted medical license by September 1st of their exam year. Failure to meet these internal board deadlines has a domino effect: if they cannot sit for the boards, they cannot achieve board-certified status, which is a requirement for many premium commercial payer contracts. Tele-Neurology and Multi-State Expansion Challenges The expansion of telestroke programs and remote EEG monitoring has transformed neurology into a borderless specialty. However, this clinical freedom creates an administrative burden. If your practice provides neurology services across state lines, you must enroll the provider in the Medicaid and commercial panels of every state where the patient is located. Enrollment in one state does not grant automatic privileges in another. Many payers now require separate telehealth-specific enrollment forms or specific modifiers to be tied to the provider’s NPI. Managing these multi-state requirements is a logistical challenge that can overwhelm internal billing departments. For practices looking to scale their remote services, we recommend studying our insights on mastering multi-state Medicaid provider enrollment. Image Description: A high-resolution photo of a professional medical administrator in a clean, modern clinical setting, reviewing digital provider profiles on a tablet with a neurology brain scan visible in the background. The High Cost of Enrollment Inertia What happens when you don’t act? The consequences of delayed neurology enrollment are far-reaching and often permanent. Unlike some errors that can be fixed retroactively, many payers do not allow for backdated effective dates. If your provider starts seeing patients on June 1st, but your enrollment application isn’t approved until August 1st, those 60 days of specialized neurology consults represent a total loss of revenue. Consider these real-world impacts on your neurology practice: Denied Claims and Revenue Loss: High-complexity codes for EMGs, nerve conduction studies, and Botox
How to Credential Nephrology Providers in 2026
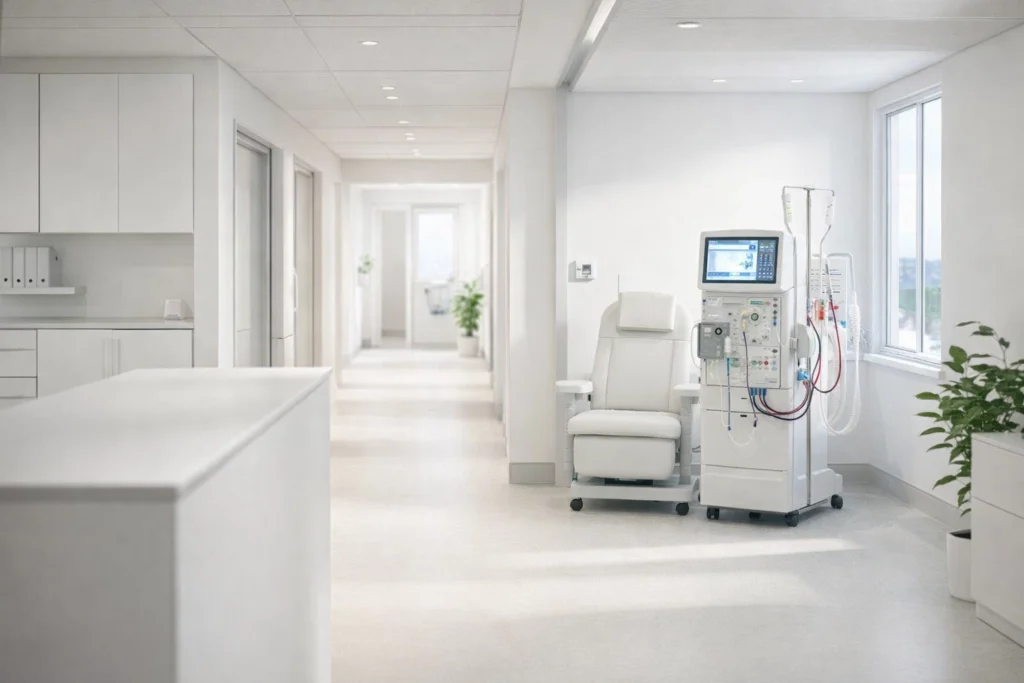
The landscape of renal care is shifting rapidly as we move through 2026. For medical practices and health systems, understanding how to credential nephrology providers is no longer a back-office administrative task; it is a critical strategic imperative. Nephrology is a high-stakes specialty where delays in payer enrollment do not just result in administrative headaches: they lead to massive revenue leakage and interrupted care for vulnerable End-Stage Renal Disease (ESRD) patients. In 2026, the complexity of this process has intensified due to enhanced federal monitoring and stricter payer requirements regarding dialysis facility privileges. If your organization is not proactive, the 120-day wait for a Provider Transaction Access Number (PTAN) will be the least of your concerns. You must master the nuances of primary source verification and the specific demands of the American Board of Internal Medicine (ABIM) to keep your revenue cycle fluid. The Foundation: Verifying Nephrology-Specific Qualifications The path to successful enrollment begins with a meticulous audit of the provider’s academic and professional history. Unlike general internal medicine, nephrology requires a secondary layer of validation that payers scrutinize with extreme prejudice. To ensure a seamless transition into your network, you must verify: Internal Medicine Board Certification: The provider must hold an active certification through the ABIM. Nephrology Subspecialty Certification: In 2026, payers are increasingly requiring direct verification codes from the ABIM to confirm the subspecialty status of the provider. Fellowship Verification: You must perform primary source verification of the provider’s completion of an ACGME-accredited nephrology fellowship. This requires direct communication with the training institution. State Licensure: An unrestricted medical license in every state where the provider will treat patients via telehealth or in-person is mandatory. Style: Minimalist architectural photography of a modern medical office building at dusk, emphasizing clean lines and professional stability. Failure to document these items before submission will result in an immediate “return to sender” from major payers. At The Veracity Group, we emphasize that a clean CV is your passport to success. Any gap in work history exceeding 30 days must be explained in writing, or the application will stall in the committee review phase. Navigating Dialysis Facility Privileges and Payer Contracts One of the most significant hurdles in learning how to credential nephrology providers is the integration of dialysis facility privileges. Nephrologists rarely practice solely within a clinic; their revenue is tied to hospital rounds and outpatient dialysis centers. In 2026, payers like UnitedHealthcare and Aetna require proof of active privileges at a Medicare-certified dialysis facility before they will finalize a provider’s enrollment under a group contract. This is particularly relevant when managing medical group enrollment for surgery centers or specialized renal clinics, where compliance risks are magnified. When submitting your applications, you must include: The facility’s CMS Certification Number (CCN). Verification of the provider’s role (Medical Director vs. Attending). Specific billing codes for ESRD services, such as CPT 90960 (Monthly Capitated Payment), to ensure the payer correctly links the provider to the appropriate fee schedule. By securing these privileges early, you avoid the common “pend” status that plagues many renal practices. Our team at Veracity ensures that every contracting detail is handled with precision to prevent these specific specialty roadblocks. 2026 Enhanced Monitoring: The New Standard As of January 1, 2026, the Department of Health and Human Services (HHS) has implemented Enhanced Monitoring Standards for all high-utilization specialties, including nephrology. The era of “set it and forget it” enrollment is over. Style: High-end corporate gradient aesthetic showing a close-up of a digital tablet displaying medical data visualizations. The new standards mandate several key activities that you must integrate into your workflow: Monthly OIG Exclusion Screening: You must screen every provider against the OIG’s List of Excluded Individuals/Entities (LEIE) and the System for Award Management (SAM) database every 30 days. Continuous License Monitoring: Rather than checking licenses at the time of re-enrollment, 2026 standards require automated tracking of license status to detect any disciplinary actions in real-time. Directory Accuracy (No Surprises Act): Under current regulations, you are required to verify provider directory information every 90 days. For nephrology, this includes confirming which dialysis centers the provider is currently servicing. If your practice fails these audits, the financial consequences are severe: claim denials, recoupments, and potential removal from the payer network. To understand the depth of these requirements, many groups find it helpful to perform a deep dive into CAQH and Medicare enrollment to see how these systems now talk to one another in real-time. The Primary Source Verification (PSV) Workflow To maintain the backbone of professional credibility, your PSV process must be beyond reproach. In 2026, payers no longer accept self-reported data for critical milestones. You must go directly to the source. Step 1: CAQH ProView and NPPES The CAQH ProView portal remains the central hub for commercial payers. You must ensure the nephrology subspecialty is accurately reflected and that all global attestations are current. Simultaneously, the National Plan and Provider Enumeration System (NPPES) must be updated to reflect the correct taxonomy codes (e.g., 207RN0300X for Nephrology). Step 2: PECOS and Medicare Enrollment For nephrology providers, Medicare is often the primary payer due to the ESRD program. Use the PECOS (Provider Enrollment, Chain, and Ownership System) to submit the 855I or 855R forms. In 2026, the Centers for Medicare & Medicaid Services (CMS) has streamlined the digital signature process, but the documentation requirements for fellowship and board status remain stringent. Step 3: NPDB Queries A formal query of the National Practitioner Data Bank (NPDB) is mandatory. This report identifies any malpractice history or adverse actions that haven’t been self-disclosed. If a provider has a history of litigation, you must provide a narrative explanation and the final settlement documents to the payer’s credentialing committee. Style: Professional still life of a high-quality stethoscope resting on a clean, modern workstation with a blurred medical certification in the background. Timelines: The High Cost of Delays Time is money, but in nephrology enrollment, time is also patient access. On average, the process of how to credential nephrology providers
How to Credential Neurosurgery Providers in 2026
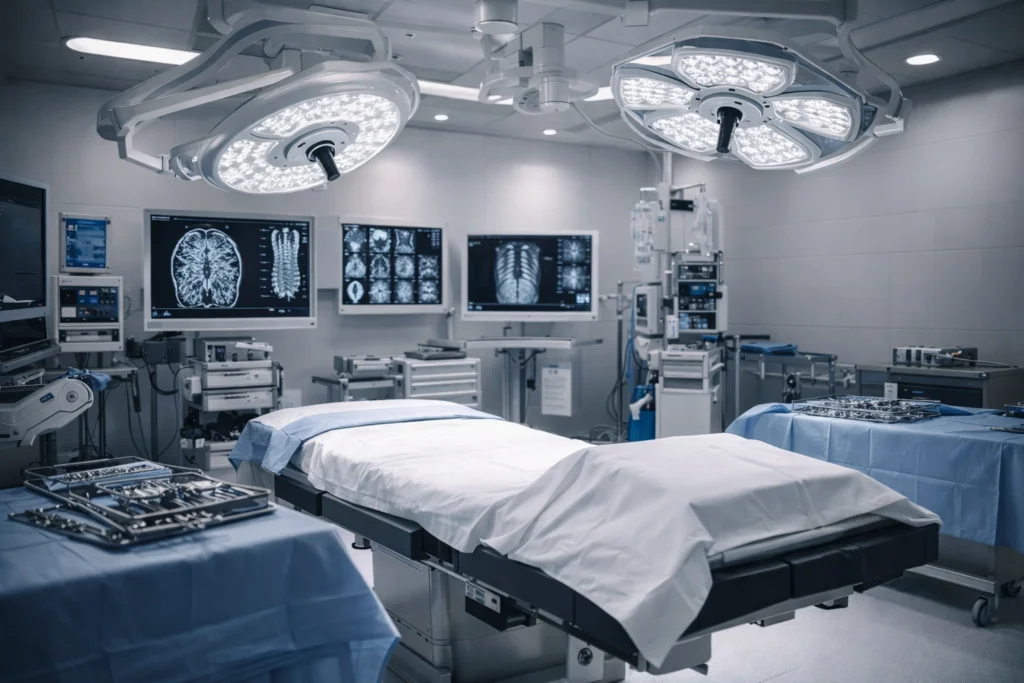
AIOSEO Title: How to Credential Neurosurgery Providers in 2026 Meta Description: Master the 2026 process for how to credential neurosurgery providers. Ensure ABNS compliance and navigate tight NCQA timelines with The Veracity Group. In the high-stakes world of neurological surgery, delays in provider enrollment are more than just administrative hurdles: they are significant financial liabilities. As we navigate the healthcare landscape of 2026, the complexity of securing network participation for neurosurgeons has intensified. Whether you are managing a private practice, a multi-specialty group, or an ambulatory surgery center, understanding how to credential neurosurgery providers is the backbone of your revenue cycle. Neurosurgery is a field defined by precision and high-value procedures. When a surgeon is unable to bill for complex cases, such as a craniotomy (CPT 61312) or the placement of a ventricular catheter (CPT 61107), the lost revenue can reach tens of thousands of dollars per week. To maintain a healthy bottom line, your organization must adopt a proactive, rigorous approach to the enrollment process. The Essential 2026 Documentation Checklist The foundation of a successful enrollment application lies in the meticulous gathering of data. In 2026, payers have zero tolerance for “pending” documents or expired certifications. For neurosurgery, the requirements are uniquely stringent due to the high-risk nature of the specialty. To begin the process, you must secure the following: ABNS Board Certification: Verification from the American Board of Neurological Surgery is mandatory. Providers must demonstrate they have completed an ACGME-accredited residency and passed all relevant examinations. State Medical License: A current, unrestricted license in every state where the surgeon will practice. DEA and CDS Registrations: Necessary for the prescription of controlled substances required in post-operative care. Malpractice Insurance: Detailed certificates of insurance (COI) showing coverage limits appropriate for neurosurgical risks (typically higher than primary care limits). Work History: A full, chronological account of the last 10 years of practice, with any gaps exceeding 30 days clearly explained. Hospital Affiliations: Documentation of where the provider currently holds or is applying for surgical privileges. Style: Modern Isometric – A clean, 3D isometric view of a modern neurosurgery office with digital filing systems and medical equipment. Navigating the Compressed 2026 NCQA Timelines A major shift in 2026 is the reduction in processing windows mandated by the National Committee for Quality Assurance (NCQA). The standard “90-day wait” is a thing of the past; organizations are now under immense pressure to complete reviews faster while maintaining higher verification standards. Currently, accredited organizations have only 120 days to finalize the process, while certified organizations must complete it within 90 days. For a specialty as complex as neurosurgery, where peer references and surgical logs must be scrutinized, this shorter window leaves no room for error. If your documentation is incomplete upon submission, the “clock” does not stop; the payer may simply reject the file, forcing you to start from scratch. This is why medical group enrollment for surgery centers requires such specialized attention to compliance risks. The Digital Foundation: CAQH and NPPES The Council for Affordable Quality Healthcare (CAQH) remains the centralized nervous system of provider data. In 2026, keeping a CAQH profile in “Initial” or “Re-attestation” status is not enough; the profile must be meticulously mapped to the provider’s NPPES (National Plan and Provider Enumeration System) data. When you learn how to credential neurosurgery providers, you quickly realize that discrepancies between CAQH and NPPES are the leading cause of “silent” denials. Payers use automated scripts to cross-reference these databases. If the neurosurgeon’s taxonomy code for “Neurological Surgery” is missing or if the practice address differs by even a suite number, the application will stall. You can find more detail on this synchronization in our deep dive into CAQH and Medicare enrollment. Primary Source Verification: The Non-Negotiable Step You cannot rely on a CV or a copy of a diploma. Primary Source Verification (PSV) is the process of contacting the issuing institution directly to confirm a provider’s credentials. For neurosurgery, this includes: Medical School and Residency: Direct contact with the registrar to confirm graduation and completion of residency. Board Status: Real-time API checks with the ABNS. National Practitioner Data Bank (NPDB): A mandatory query to check for any history of malpractice payments or adverse actions. The Veracity Group utilizes advanced workflows to automate these checks, but the human element remains vital. In 2026, many institutions have moved to third-party verification hubs which require specific release forms signed by the surgeon. Failure to provide these releases on day one will result in avoidable delays. Style: Modern Isometric – An illustration showing a secure data flow from a medical board to a provider’s digital profile. Clinical Privileges and Hospital Integration Neurosurgery is rarely practiced in a vacuum. Most surgeons require hospital or ASC privileges to perform their work. In 2026, the integration between hospital privileging and payer enrollment has become more intertwined. Many payers now require proof of “Active” hospital status before they will issue a provider ID. This “chicken and egg” scenario can be a nightmare for new hires. You must coordinate the hospital’s medical staff office (MSO) timeline with your payer enrollment submissions. If the hospital takes 60 days to grant privileges, but the payer requires that approval up front, you are looking at a minimum of five months before that surgeon can see an insured patient. Managing these parallel tracks is the hallmark of an expert enrollment strategy. The High Cost of Enrollment Delays Why is the urgency so high? Consider the impact on a neurosurgery practice’s revenue. When a provider is not yet “in-network,” patients are often redirected to competitors, or the practice is forced to accept “out-of-network” rates that barely cover the overhead of a surgical suite. Furthermore, claims recycling: the practice of holding claims until a provider is loaded into the system: is a risky gamble. In 2026, many payers have shortened their timely filing windows. If the enrollment process drags on past 120 days, you may find that your oldest claims are no longer eligible for reimbursement, regardless of

