How to Credential Vascular Surgery Providers in 2026

In the high-stakes world of Vascular Surgery, precision is not just a skill: it is a requirement. Whether your practice operates independently or works in tandem with Cardiothoracic Surgery departments, the administrative burden of onboarding can often feel like a bottleneck to patient care. Implementing a robust strategy for Provider Enrollment Management is the only way to ensure your surgeons are in-network and ready to operate the moment they join the team. Without proactive CAQH Management, even the most talented vascular specialist is sidelined, leading to lost revenue and delayed life-saving procedures. Utilizing professional medical provider enrollment services is the silent driver of a profitable surgical department. The High Cost of Enrollment Delays For a vascular surgeon, a single day of being out-of-network is a massive financial hit. Consider the complexity of the procedures: abdominal aortic aneurysm (AAA) repairs, carotid endarterectomies, and complex peripheral bypasses. These are high-value services that require extensive hospital resources and surgical support. If your enrollment is not finalized, you cannot bill for these services, and the facility fees alone can create a massive deficit. The silent driver of practice failure is often found in the “pending” pile of a payer’s desk. When a provider joins a group, the assumption is often that they can begin seeing patients immediately. However, the reality of the American healthcare system is that payers can take 90 to 180 days to process an application. For a high-volume specialty like vascular surgery, that timeline is unacceptable. You must utilize expedited pathways and delegated agreements to bypass these traditional roadblocks. A minimalist 3D render of a human circulatory system in glowing blue and silver tones, representing the precision of vascular medicine. Navigating Specialty-Specific Requirements Vascular surgery is unique because of its heavy reliance on diagnostic imaging and office-based labs (OBLs). Enrollment isn’t just about the surgeon; it is about their ability to bill for the interpretation of the tests they perform. RPVI Certification: Most major payers now require the Registered Physician in Vascular Interpretation (RPVI) credential to reimburse for vascular ultrasound. If your enrollment packet does not prominently feature this certification, your “global” billing for the OBL will be denied, leaving you with only the technical component: or nothing at all. Hospital Privileging and Medicare: You cannot successfully complete Medicare enrollment without verified hospital privileges for the specific facilities where you will perform inpatient work. The Centers for Medicare & Medicaid Services (CMS) maintain strict standards for surgical specialties, and any discrepancy between your PECOS application and your hospital’s medical staff office records will result in an immediate rejection. The Hybrid Suite Factor: As more vascular procedures move to hybrid suites and ambulatory surgery centers (ASCs), the complexity of your medical group enrollment for surgery centers increases. Each location requires specific NPI Type 2 links that must be established during the initial enrollment phase. The Blueprint for Speed: Strategic Steps To achieve fast provider enrollment, you cannot simply submit an application and wait. You must be aggressive. The process is a “passport to success” that requires a methodical approach to documentation. Gathering the Core Essentials Before you even open a payer portal, your digital “war chest” must be ready. This includes: A current medical license with at least six months of future validity. Board certifications (ABMS or AOA). A comprehensive 10-year work history with no gaps. Current professional liability insurance (Malpractice) that meets the high-limit requirements typical for surgical specialties. The Power of CAQH Your CAQH profile is the backbone of professional credibility in the digital age. It must be updated and re-attested every 120 days. Many delays occur simply because a provider’s CAQH state is “Incomplete” or “Expired.” For vascular surgeons, ensuring that your sub-specialty designations are correctly coded is vital for appearing in the correct patient directories. You can learn more about navigating the maze of CAQH and Medicare enrollment to avoid common pitfalls. A high-end, clean corporate office setting with a sleek glass desk and a digital tablet showing synchronized medical data. Leveraging Delegated Enrollment One of the most effective ways to accelerate the timeline is through delegated enrollment agreements. This occurs when a large medical group or a professional service provider has an agreement with a payer to perform the vetting process themselves. Instead of the payer spending months verifying your surgical background and education, they trust the delegated entity’s report. This can cut the “wait time” from six months down to as little as 30 days. For a vascular practice looking to expand into a new territory, this is the difference between a successful launch and a financial disaster. Common Roadblocks for Vascular Specialists Even with the best preparation, certain obstacles are inherent to the specialty. Being aware of them allows you to navigate around them before they become a crisis. Multi-State Licensure: Many vascular surgeons operate across state lines, particularly in metropolitan areas that span several borders. Mastering multi-state Medicaid provider enrollment is a specialized skill. Each state has different requirements for background checks and site visits. The “OBL” Trap: If you are moving from a hospital-employed model to an office-based lab model, your enrollment status does not automatically follow you. You are essentially a “new” provider in the eyes of the payer’s billing system. Coding Changes: Billing codes for vascular procedures (like those in the 37000 series) are frequently updated. If your enrollment is tied to an outdated NPI profile or an incorrect taxonomy code, your claims for endovascular repairs will be stuck in “limbo” indefinitely. A professional close-up of a vascular surgeon’s hands with high-quality lighting, highlighting precision and modern technology. Why Outsourcing Is the New Standard The complexity of modern healthcare administration means that a “DIY” approach to enrollment is no longer viable for high-acuity specialties. The Society for Vascular Surgery (SVS) often highlights the administrative burden placed on modern surgeons. By using professional medical provider enrollment services, you are not just “outsourcing paperwork”: you are protecting your revenue cycle. A dedicated enrollment team understands the nuances of the “Vascular” taxonomy codes.
How to Credential Vision Providers in 2026

For Ophthalmology clinics and independent Optometrists, the path to a profitable practice begins long before the first comprehensive eye exam is ever performed. Ensuring your practice remains financially viable requires a rigorous focus on CAQH Management and comprehensive Provider Enrollment Management to avoid the pitfalls of modern healthcare administration. When your enrollment process is delayed, your revenue cycle stalls, creating a ripple effect that impacts patient care and staff morale. Utilizing expert medical provider enrollment services is no longer a luxury: it is the backbone of a successful vision care operation in an increasingly competitive market. The Administrative Burden of Vision Care Vision care is a unique beast in the healthcare world. Unlike general practitioners, vision specialists must navigate a dual-layer system of both medical insurance and vision benefit plans. This complexity means that a single provider often needs to be credentialed with dozens of different entities, from major medical carriers like Blue Cross Blue Shield to vision-specific giants like VSP and EyeMed. The administrative side of things is the engine under the hood. If that engine isn't tuned, the whole car stops moving. Many practices treat enrollment as a "set it and forget it" task, but in 2026, this passive approach is dangerous. Proactive management is the only way to avoid the high cost of delays. A single missing signature or an outdated CAQH profile can result in months of "out-of-network" status, forcing you to either turn patients away or eat the cost of the services rendered. Style: A clean, high-end 3D render of a futuristic human eye with digital data streams orbiting the iris, representing the intersection of vision care and data management. Minimalist white background. Why Enrollment is the Silent Driver of Your Revenue In the vision industry, your ability to bill for specific codes: such as 92002 or 92004 for ophthalmological services: is entirely dependent on your enrollment status. If you aren't properly linked to the payer, those claims will bounce faster than a rubber ball. Eliminating the "Pending" Trap: New providers often wait 90 to 120 days to be fully loaded into payer systems. Professional medical provider enrollment services can often shave weeks off this timeline by ensuring applications are "clean" the first time they are submitted. Capturing Medical vs. Routine Billing: Vision practices live in the gray area between routine exams and medical eye care (glaucoma, cataracts, macular degeneration). You must be correctly enrolled in both medical and vision panels to capture the full scope of your billable work. Maintaining Patient Loyalty: Nothing kills a patient relationship faster than a surprise bill because their "covered" exam was rejected due to an enrollment technicality. To stay ahead of these issues, it is essential to understand that enrollment matters, especially when regulatory changes shift the landscape of how vision benefits are processed. Navigating the "Big Three" of Vision Enrollment For most vision practices, the "Big Three" are Medicare, VSP, and EyeMed. Each has its own set of rules, portals, and "hoops" that you must jump through. 1. Medicare Enrollment (CMS) Medicare is the foundation for any practice treating geriatric patients or medical eye conditions. Whether you are an ophthalmologist performing surgery or an optometrist managing chronic conditions, your Medicare enrollment must be airtight. Medicare requires strict adherence to PECOS (Provider Enrollment, Chain, and Ownership System) updates and revalidations every five years (or three years for DMEPOS). 2. VSP and EyeMed These are the gatekeepers of vision care. Unlike medical insurance, vision plans often have "closed panels," meaning they may not be accepting new providers in your specific zip code. You must demonstrate a need for your services in that area or have a unique specialty (like low vision or pediatric optometry) to break through. This is where professional contracting expertise becomes your greatest asset. 3. CAQH Management Think of CAQH as your professional passport. If your passport is expired, you aren't going anywhere. For vision providers, CAQH management involves quarterly attestations and the constant uploading of current malpractice insurance, state licenses, and DEA certificates (where applicable). Even a 24-hour lapse in attestation can trigger a suspension of your insurance payments. Style: A minimalist, corporate editorial photograph of a modern, white-space-heavy optometry clinic. Sharp focus on high-end diagnostic equipment with a blurred, professional background. The Digital Shift: Automation and Pre-Registration According to the American Optometric Association, modernizing the patient intake process is one of the most effective ways to reduce administrative friction. By implementing digital pre-registration tools, you can collect insurance data before the patient ever steps into the exam lane. This data allows your staff to perform real-time eligibility checks. If you discover a provider enrollment issue during this phase, you can address it before a claim is even generated. It transforms your front office from a "reactive" department into a "proactive" one. Common Pitfalls for Vision Groups Whether you are a solo practitioner or a multi-location group, certain mistakes will cost you. As we’ve outlined in our guide on common credentialing mistakes, the consequences of oversight are severe. Failure to Update Demographics: Did you move suites? Change your phone number? If your demographic updates aren't synced across all payers, your checks will be sent to the wrong address, or worse, your contract will be terminated for "undeliverable" mail. Ignoring Multi-State Requirements: If you are a vision group expanding across state lines, you must navigate the nightmare of multi-state Medicaid enrollment. Each state has its own unique portal and background check requirements. The "New Hire" Lag: Bringing on a new associate is exciting, but if you don't start their provider enrollment process at least 90 days before their start date, they will be sitting in an exam room unable to generate revenue. Style: Modern digital 3D render of interconnected nodes and glowing light paths, symbolizing the complexity of multi-state healthcare networks and data integration. High-contrast, clean aesthetic. Implementing a Solution that Works The goal of any vision practice is to provide exceptional eye care, not to become an expert in insurance bureaucracy. However, the reality
How to Credential Surgery Providers in 2026

In the high-stakes environment of 2026 healthcare, surgical departments remain the primary revenue engines for hospitals and multi-specialty groups. However, that engine stalls the moment a surgeon is unable to bill for their procedures. Surgery provider enrollment is no longer a “set it and forget it” administrative task; it is a complex, high-velocity requirement that demands precision, clinical data alignment, and proactive management. When a surgeon joins your team, the clock starts ticking. Every day they spend in the operating room without active payer enrollment represents tens of thousands of dollars in uncollectible revenue. To thrive in the current landscape, your organization must adopt a rigorous approach to medical provider enrollment services that accounts for the unique complexities of surgical specialties. The Surgical Enrollment Landscape in 2026 The year 2026 has introduced a shift toward continuous monitoring and real-time data validation. Payers are no longer satisfied with periodic re-attestations every few years. Instead, they are utilizing automated systems to cross-reference state board actions, DEA registrations, and malpractice databases daily. For surgery providers, whose liability profiles and procedural volumes are under constant scrutiny, this means the margin for error is non-existent. To ensure your surgeons are ready to operate and receive reimbursement, you must understand the interplay between board certification, hospital privileges, and payer-specific requirements. Alt Tag: Corporate gradient visual of sterile surgical instruments, emphasizing the meticulous nature of surgery provider enrollment services. The Core Documentation: Your Surgeon’s “Passport” Before initiating any application, you must compile a comprehensive digital “passport” for the provider. In 2026, incomplete documentation is the leading cause of “pended” applications, which can delay enrollment by months. Essential documentation for surgery provider enrollment includes: Current State Medical Licenses: Ensure the surgeon holds an active license in every state where they will perform procedures. Board Certification (ABS or Specialty Specific): Payers prioritize providers who maintain active status with the American Board of Surgery (ABS). In 2026, board eligibility is often insufficient for top-tier payer contracts; full certification is the gold standard. DEA and CSR Registrations: These must match the primary practice address to avoid pharmacy and billing flags. Malpractice Insurance (COI) and Loss Runs: Surgeons face intensive review of their malpractice history. You must provide a 10-year history of “loss runs” or claim histories, even if those claims were dismissed. Procedural Case Logs: This is a 2026-specific priority. Payers frequently request the last 12–24 months of surgical case volumes to ensure proficiency in the procedures being billed. Specialty-Specific Requirements: Beyond the Basics Surgery is not a monolithic field. The requirements for a general surgeon differ significantly from those in highly specialized niches. If your group is expanding into other areas, you may need to look at our specific guides for neurosurgery providers or orthopedic surgery providers to understand the unique procedural nuances involved in those enrollments. The Role of the American College of Surgeons (ACS) The American College of Surgeons (ACS) sets the bar for surgical excellence. While ACS fellowship (FACS) is a prestigious designation, payers in 2026 increasingly use ACS standards to verify a surgeon’s commitment to ongoing education and clinical safety. Highlighting a surgeon’s FACS status in the enrollment application can often streamline the committee review process, as it serves as a pre-verified mark of quality. Case Volumes and Peer Review In 2026, “minimum volume” requirements are a reality. Payers have become more aggressive in denying enrollment for specific high-risk CPT codes if the surgeon cannot prove they have performed a sufficient number of those procedures in the preceding year. This makes medical provider enrollment services a data-driven exercise. You must be prepared to submit peer references: specifically from other surgeons or department chairs: who can attest to the provider’s clinical outcomes and technical skills. Navigating the CAQH ProView and PECOS Maze The CAQH ProView profile remains the backbone of professional credibility for surgeons. However, simply having a profile is not enough. 90-Day Attestation: In 2026, failing to re-attest every 90 days results in an immediate “inactive” status, which can trigger a cascade of claim denials. Document Accuracy: Every address, from the surgical center to the satellite clinic, must be listed and matched exactly with the provider’s NPI (National Provider Identifier) record. Medicare Enrollment (PECOS): For surgical centers and groups, Medicare enrollment via PECOS is a critical hurdle. Any discrepancy between the surgeon’s individual Type 1 NPI and the group’s Type 2 NPI will result in a rejected application. For a deeper understanding of how these systems interact, our guide on navigating the maze of CAQH and Medicare enrollment provides a detailed roadmap for administrative success. The High Cost of Enrollment Delays The financial consequences of a botched surgery provider enrollment are staggering. Consider a scenario where a general surgeon joins a practice with a projected monthly revenue of $200,000. If the enrollment process is delayed by 60 days due to a missing malpractice loss run or an unverified hospital privilege, the practice loses $400,000 in gross charges. Most of this revenue is unrecoverable, as payers rarely offer retroactive reimbursement for surgical services performed prior to the effective date of enrollment. Consequences of inefficient enrollment include: Revenue Leakage: Thousands of dollars in written-off claims. Operational Friction: Surgeons who are “ready to work” but are legally and financially unable to see patients. Patient Dissatisfaction: Delayed surgeries due to insurance “out-of-network” status. Compliance Risks: Operating without proper payer-verified credentials can lead to audits and “clawbacks” of previously paid claims. Strategies for Success in 2026 To avoid these pitfalls, The Veracity Group recommends a proactive, three-tier strategy for all surgical practices: 1. Pre-Boarding Initiation Start the enrollment process the moment the employment contract is signed: ideally 90 to 120 days before the surgeon’s start date. Do not wait for the surgeon to move to your city or finish their fellowship. Early data collection is the only way to combat the 2026 backlog in primary source verification. 2. Hospital Privilege Alignment Ensure that the surgeon’s hospital privileges align exactly with the payers you are targeting. If a payer sees that
How to Credential Occupational Therapy Providers in 2026

The landscape of healthcare reimbursement is shifting beneath the feet of providers. As we move through 2026, Occupational Therapy credentialing is no longer a “set it and forget it” administrative task; it is the backbone of professional credibility and the silent driver of your practice’s financial health. For therapy practices, the stakes have never been higher. A single oversight in the enrollment process does not just delay a start date: it triggers a cascade of claim denials that can jeopardize months of revenue. To succeed in this environment, your practice must treat enrollment as a strategic priority. Whether you are onboarding a new graduate or a seasoned clinician, understanding the current regulatory demands is the only way to ensure your facility remains compliant and profitable. The 2026 Standard: Accelerated Timelines and Stricter Compliance The most significant change facing providers this year is the compression of the verification window. Historically, organizations had a 180-day cushion for primary source verification (PSV). As of late 2025, that window has tightened. For all files handled in 2026, primary source verification must be completed within 120 days. This 60-day reduction means your administrative team: or your chosen medical provider enrollment services: must operate with surgical precision. There is zero room for the “wait and see” approach. If a verification of education or licensure hits a snag, you no longer have the luxury of time to correct it before the file expires. Furthermore, compliance checks have become more aggressive. Payers are now performing real-time exclusion monitoring against Medicare and Medicaid databases. If an OT provider has even a minor sanction that hasn’t been properly cleared, your entire group’s enrollment status could be flagged for a deep-dive audit. Navigating NBCOT and AOTA Requirements Every qualified Occupational Therapist (OT) and Occupational Therapy Assistant (OTA) must satisfy rigorous national standards before they can even be considered for payer enrollment. In 2026, the focus on continuous certification is paramount. NBCOT Certification: All providers must have successfully passed the NBCOT (National Board for Certification in Occupational Therapy) exam. While some states allow practice without maintaining active NBCOT status after initial licensure, many high-value insurance payers require “Active” status for preferred provider tiering. ACOTE Accreditation: Verification must confirm the provider graduated from an ACOTE-accredited occupational therapy program. This is the “passport to success” in the credentialing world; without this foundational verification, enrollment stops dead. Professional Development Units (PDUs): Maintaining credentials now requires a strict adherence to a 3-year cycle, necessitating 36 professional development units. Payers are increasingly asking for proof of these units during re-credentialing cycles to ensure the provider is current on adaptive technology and modern therapeutic interventions. The American Occupational Therapy Association (AOTA) continues to set the standard for ethical practice and continuing education. Aligning your practice’s internal standards with AOTA’s 2026 guidelines is not just good clinical sense: it is a defensive maneuver against payer scrutiny. The OT Licensure Compact: A Passport to Multi-State Practice For practices located near state borders or those utilizing telehealth to reach underserved populations, the OT Licensure Compact is a game-changer. In 2026, more states than ever have joined the compact, allowing licensed OTs to practice in member states without the grueling process of obtaining ten separate licenses. However, the “Compact Privilege” does not automatically grant you enrollment with local payers. You must still navigate state-specific Medicaid requirements and local commercial payer contracts. This is where many practices stumble. They assume a compact license means an automatic “green light” for billing. In reality, you must still submit individual enrollment applications for each state’s Medicaid program if you intend to treat those beneficiaries. Much like the complexities we see in Physical Therapy or the specialty-specific demands of PM&R, Occupational Therapy requires a nuanced approach to state-by-state variations. Essential Specialty Codes and Documentation Occupational Therapy is unique because of its focus on “functional” outcomes. Payers in 2026 are looking for specific documentation that justifies the use of specialty CPT codes. If your provider is not properly credentialed and linked to your NPI, claims for the following will be rejected instantly: 97110: Therapeutic Procedure (Strength and endurance) 97530: Therapeutic Activities (Dynamic activities to improve functional performance) 97535: Self-care/Home Management Training (ADL training and adaptive equipment) Beyond the codes, the Occupational Therapy credentialing process must verify that the provider is qualified to use specific modalities. For example, if your OT specializes in hand therapy or lymphedema, those certifications must be primary-source verified and uploaded to the CAQH ProView portal. Failure to do so will result in “carve-outs” where the payer approves the provider for general therapy but denies them for specialized, higher-reimbursement procedures. Avoiding the Revenue Trap: Common Enrollment Pitfalls The “High Cost of Delay” is a phrase we use often at The Veracity Group because we see the consequences daily. A provider who is seeing patients but isn’t yet “par” (participating) with a payer is essentially working for free. Worse, they are creating a legal liability for the practice. Common pitfalls include: Gaps in Practice: For providers who have been out of the workforce for 3 to 8 years, many state boards and payers now require “re-entry” documentation and additional contact hours. Expired CAQH Profiles: If the CAQH profile is not re-attested every 90 days, payers will drop the provider from their directories. A patient searching for an OT may see “Not Accepting New Patients” or find the provider missing entirely, leading to a direct loss of market share. Incomplete Demographic Updates: If your practice moves or adds a new location, demographic updates must be filed immediately. Billing from an unlinked location is a leading cause of the “Claim Not Found” or “Provider Not Enrolled at This Location” denial codes. Why Specialized Medical Provider Enrollment Services Are Critical The complexity of healthcare in 2026 has outpaced the capacity of most in-house billing departments. Managing the nuances of multi-state Medicaid while simultaneously tracking NBCOT renewals and 120-day PSV deadlines is a monumental task. By utilizing professional medical provider enrollment services, you shift the burden of administrative “perfection”
How to Credential Rheumatology Providers in 2026

In the high-stakes landscape of 2026, Rheumatology enrollment is no longer a back-office administrative task; it is the financial backbone of your practice. As the healthcare industry shifts toward tighter regulatory oversight and value-based reimbursement models, the margin for error in provider enrollment has vanished. For rheumatology groups, where high-cost biologic infusions and long-term chronic disease management are the norms, a single gap in enrollment can lead to devastating revenue leakage and interrupted patient care. The complexity of Rheumatology stems from its intersection with various medical disciplines. Because most providers in this field are dual-certified, the enrollment process often mirrors the rigorous standards found in Internal Medicine provider enrollment. However, 2026 introduces specific hurdles that require an insider’s perspective to clear. At The Veracity Group, we have seen how meticulous preparation acts as a passport to success in an increasingly scrutinized market. The 2026 Regulatory Landscape for Rheumatology The year 2026 marks a turning point in how CMS and private payers evaluate specialists. We are seeing an unprecedented level of enhanced background screening. Effective January 1, 2026, CMS has implemented stricter fingerprint-based background checks for various provider categories and mandated monthly sanctions screening against the OIG exclusion list and the System for Award Management (SAM) database. For a rheumatology practice, this means your medical provider enrollment services must be proactive rather than reactive. If a provider’s credentials lapse for even twenty-four hours, the automated systems used by major payers like UnitedHealthcare and Anthem will flag the account, potentially triggering an immediate suspension of payments. Image Alt Tag: Earth-tone minimal healthcare graphic on textured paper with abstract network lines and a subtle hand/joint outline, representing accurate rheumatology enrollment. Board Certification and Specialty Requirements A successful enrollment begins with the American Board of Internal Medicine (ABIM). To be recognized as a specialist in rheumatology, a physician must first maintain their certification in internal medicine and then complete a certified fellowship to pass the Rheumatology Certification Examination. Payers in 2026 are increasingly verifying these credentials through real-time API links with the ABIM. Any discrepancy in name spelling, certification dates, or fellowship documentation will result in an immediate “Return to Provider” (RTP) status. Furthermore, the American College of Rheumatology (ACR) sets clinical standards that many private payers now use as a benchmark for network inclusion. Being an active member and adhering to ACR-recognized quality metrics can significantly smooth the path during the initial contracting phase. Navigating the PECOS and CAQH Maze The “silent driver” of your practice’s cash flow is the Provider Enrollment, Chain, and Ownership System (PECOS). In 2026, using the CMS-855I form for individual practitioners requires more than just basic information. You must provide: Detailed Work History: A comprehensive 10-year history with no gaps. Any period of unemployment exceeding 30 days must be explained in writing. Malpractice Coverage: Declarations pages showing a clean 10-year history. Payers are now scrutinizing the “tail” coverage more closely than ever. Specialty-Specific Equipment: If your practice operates an in-house infusion suite or uses high-resolution musculoskeletal ultrasound, these must be disclosed and correctly linked to your NPI. Because rheumatology involves complex metabolic interactions, our team often notes that the precision required here is similar to the standards seen in Endocrinology provider enrollment. Missing a single disclosure regarding ownership or site-specific billing can delay your “effective date” by months, costing the practice hundreds of thousands in unreimbursed biologic treatments. The High Cost of Enrollment Delays In rheumatology, the cost of a delay is exponentially higher than in primary care. Consider the billing of J-codes for biologics such as adalimumab, rituximab, or infliximab. These drugs represent a massive upfront investment for the practice. If your Rheumatology enrollment is not finalized, or if your provider is not correctly linked to the group’s NPI for the specific site of service, payers will deny these high-dollar claims. There is no “retroactive magic” that can fix a failure to enroll before treating a patient. If the payer deems the provider “out of network” or “unauthorized” on the date of service, the financial liability often falls entirely on the practice. This is why The Veracity Group emphasizes a “start 90 days early” rule. The typical timeline in 2026 ranges from 6 to 10 weeks for commercial payers and up to 90 days for Medicare, assuming no errors are made. Image Alt Tag: Earth-tone minimal healthcare imagery with a tablet and subtle DNA/joint icon on natural textures, showing how clean rheumatology enrollment supports financial stability. Quality Metrics and Value-Based Care in 2026 For the first time, MIPS scores and value-based care metrics are factoring directly into enrollment decisions. Medicare Advantage plans and narrow-network commercial products are now reviewing patient outcome data and satisfaction scores during the initial credentialing phase. If a provider’s MIPS score falls below the 2026 thresholds, payers may deny entry into their “Gold Tier” or “Preferred” networks. This directly impacts your ability to attract patients and negotiate favorable rates. Professional medical provider enrollment services now include a review of these metrics to ensure the provider is presented in the best possible light to the credentialing committee. Critical Documentation Checklist To avoid the “rejection loop,” ensure your digital “credentialing vault” contains the following verified documents: State Medical Licenses: Current and unrestricted for every state where the provider sees patients (including telehealth). DEA Certificate: Must match the primary practice address. Board Certification: Verified via the ABIM portal. Hospital Privileges: Necessary if the rheumatologist performs inpatient consultations. Peer References: At least three current contacts who can attest to clinical proficiency in rheumatology specifically. Immunization Records: Meeting the updated 2026 CDC guidelines for healthcare workers. Continuous Monitoring: The New Standard The era of “set it and forget it” enrollment is over. In 2026, the industry has moved to continuous monitoring. Payers now employ automated crawlers that check state boards and OIG lists daily. At Veracity, we recommend a robust internal audit every 30 days to ensure that no licenses are approaching expiration and that all CAQH profiles are re-attested correctly. Failure to maintain your CAQH profile
How to Credential Sports Medicine Providers in 2026

The landscape of Sports Medicine credentialing is shifting rapidly as we move through 2026. With the rise of specialized athletic clinics and the integration of advanced diagnostic technologies like point-of-care ultrasound (POCUS), the requirements for bringing a new provider into your fold are more rigorous than ever. If your practice treats athletes, from the weekend warrior to the professional competitor, you know that speed and accuracy in enrollment are your backbone of professional credibility. In 2026, a “one-size-fits-all” approach to provider enrollment is a recipe for revenue leakage. Sports Medicine is inherently multi-disciplinary, drawing from Family Medicine, Physical Medicine & Rehabilitation (PM&R), and Orthopedic Surgery. Each of these pathways carries specific board certification requirements and subspecialty nuances that medical provider enrollment services must navigate with precision. Failure to align these details with payer expectations results in immediate claim denials and frustrated patients who cannot access the specialized care they need. The Multi-Disciplinary Foundation of Sports Medicine To successfully manage Sports Medicine credentialing, you must first identify the primary board path of your provider. In 2026, payers are scrutinizing the Certificate of Added Qualifications (CAQ) more than ever. This isn’t just a “nice-to-have” distinction; it is the passport to success for high-reimbursement sports medicine contracts. Family Medicine Pathway: These providers must complete an ACGME-accredited Sports Medicine Fellowship. By 2026, the American Board of Family Medicine (ABFM) requires proof of fellowship completion by specific deadlines (typically October for July exams) to sit for the subspecialty examination. PM&R (Physiatry) Pathway: Known as the “non-surgical” orthopedic experts, these providers must be diplomates in good standing with the American Board of Physical Medicine and Rehabilitation (ABPMR). The 2026 examination window for their sports medicine subspecialty is strictly regulated, and missing these dates can delay your provider’s full enrollment by a year. Orthopedic Pathway: For your surgical sports medicine providers, the American Board of Orthopedic Surgery (ABOS) remains the gold standard. Credentialing here involves verifying not just the primary surgical board, but the specific subspecialty fellowship in sports medicine. Understanding these distinctions is vital when you are coordinating with organization like the American Medical Society for Sports Medicine (AMSSM), which sets the benchmark for clinical excellence in the field. Strategic Navigation of 2026 NCQA Timelines Time is your most valuable resource, and in 2026, the National Committee for Quality Assurance (NCQA) has tightened the screws. The processing window for accredited organizations has been reduced significantly: often down to a 90-day window. This means your medical provider enrollment services must be proactive, not reactive. A delay of even two weeks in submitting a CAQH profile or a Medicare PECOS application can result in a “dark period” where your provider is seeing patients but cannot bill for them. This creates a silent driver of financial instability within the practice. To avoid this, your internal team or your external partner at The Veracity Group must initiate the process at least 120 days before the provider’s anticipated start date. High-Stakes Billing: Integrating Procedural Coding Sports Medicine is a procedure-heavy specialty. If your Sports Medicine credentialing doesn’t account for the specific procedural capabilities of your provider, you are leaving money on the table. Payers frequently trigger audits for high-frequency sports medicine codes, and the enrollment file must support the provider’s right to perform these services. Key codes that require specific credentialing focus in 2026 include: 20610 & 20611: Arthrocentesis, aspiration, or injection of a major joint. Code 20611 specifically includes ultrasound guidance and requires the provider to have documented training in POCUS. 76881 & 76882: Diagnostic ultrasound of the extremity, which requires proof of competency that many payers now demand during the initial enrollment phase. 99211-99215 with Modifier 25: Managing the office visit alongside a procedure. Your enrollment strategy must also bridge the gap between different clinical settings. For example, if your provider performs surgery, you must ensure their enrollment is synced with medical group enrollment for surgery centers to avoid compliance risks and split-billing errors. Furthermore, as many sports medicine plans involve rehabilitation, ensuring your providers are linked with the correct Physical Therapy protocols is essential for a seamless patient journey. The Revenue Bottleneck: Why Delay is Not an Option In the high-performance world of sports medicine, your reputation is built on access. A patient searching a directory who finds your provider “not in-network” will simply move to the next clinic. This is the high cost of delays. When you allow Sports Medicine credentialing to lag, you aren’t just losing the individual claim; you are losing the lifetime value of that patient and the referral source. Whether it’s a high school athletic director or a local professional team, they require their athletes to be seen by “cleared” and “covered” providers. The American College of Sports Medicine (ACSM) emphasizes the importance of the “Sports Medicine Team.” In the administrative sense, that team includes your enrollment specialists. If the specialist isn’t part of the team, the physician is essentially sidelined. Best Practices for 2026 Enrollment Success To maintain a competitive edge, your practice must implement the following “insider” strategies: Digital Repository Management: Maintain a “Live File” for every provider. This includes current ACLS/BLS certifications, updated CMEs that meet the 2026 requirements, and a clear, high-resolution copy of their DEA license with the correct address. CAQH Vigilance: In 2026, CAQH re-attestation is more frequent. Set an automated internal trigger to check CAQH status every 45 days. Any “discrepancy” flag in CAQH is a signal to payers to stop payment. The 25-Mile Rule: For providers traveling to various training camps or satellite offices, ensure their enrollment covers every physical location where they provide care. Payer “ghost locations” are a major source of 2026 audit triggers. Leveraging Expert Support with The Veracity Group Navigating the maze of healthcare regulations is daunting, but you don’t have to do it alone. At The Veracity Group, we specialize in the complexities of specialty-specific enrollment. We understand that a Sports Medicine physician isn’t just another doctor: they are a specialized asset to your clinic that requires a tailored
How to Credential Primary Care Providers in 2026

In the rapidly evolving landscape of 2026, primary care remains the front door of the American healthcare system. For medical groups and health systems, the ability to get these providers “on the glass” and seeing patients is the primary driver of organizational stability. However, primary care enrollment is not a simple administrative hurdle; it is a complex, high-stakes navigation of federal regulations, private insurance requirements, and rigorous verification standards. When a primary care physician (PCP) is unable to bill for services, the financial impact is immediate. A single provider generates significant downstream revenue, from laboratory orders to specialist referrals. Any friction in the medical provider enrollment services workflow results in leaked revenue and, more importantly, a breakdown in patient access. To thrive in 2026, you must treat enrollment as a strategic priority, not a clerical afterthought. The Foundation: Documentation and Preparation The success of your enrollment strategy begins long before a single application is submitted. In 2026, payers have tightened their requirements for “clean” data. An incomplete application or a missing document is no longer just a delay; it is an automatic rejection that resets the 90-to-120-day clock. For primary care providers, the documentation package must be exhaustive. You will need to gather: Medical diplomas and transcripts from accredited institutions. Residency completion certificates (and fellowship certificates if the PCP has a sub-specialty). Board certifications from the American Board of Internal Medicine (ABIM) or the American Board of Family Medicine. Active state medical licenses for every state where the provider will practice. DEA registration and state-specific controlled substance permits. Malpractice insurance certificates with a detailed 10-year claims history. Work history with no gaps larger than 30 days; any gaps must be explained in a formal attestation. Maintaining a centralized digital repository of these documents is the backbone of professional credibility. Without this foundation, your practice is vulnerable to significant administrative backlogs. Navigating the Digital Gatekeepers: CAQH and PECOS In 2026, the CAQH ProView profile and the Medicare PECOS system are the two most critical digital gatekeepers in healthcare. For primary care enrollment, these platforms must be perfectly synchronized. CAQH registration is the industry standard that allows commercial payers to access a provider’s data. You must ensure the provider’s profile is not only complete but re-attested every 90 days. A lapsed CAQH profile is the leading cause of “silent” claim denials, where the payer continues to process claims but withholds payment due to expired credentials in their database. Similarly, Medicare enrollment via the PECOS (Provider Enrollment, Chain, and Ownership System) requires precision. For primary care, this includes selecting the correct specialty codes and ensuring the NPI (National Provider Identifier) data matches the state license exactly. If you are managing a multi-specialty group, you should review our deep dive into navigating the maze of CAQH and Medicare enrollment to avoid common pitfalls that plague even the most experienced administrators. Alt Text: Mid-century modern geometric scene representing primary care enrollment—abstract forms, terminals, and verification symbols in a clean clinic admin setting. Primary Source Verification (PSV): The Trust but Verify Model The most time-consuming phase of the enrollment cycle is Primary Source Verification (PSV). This is where the organization or the payer independently confirms that the provider is who they say they are. In 2026, automated verification tools have sped up the process, but manual outreach to medical schools and previous employers is still common. Key elements of PSV include: Education and Training: Directly contacting the medical school and residency program to confirm graduation. Licensure: Verifying with the State Medical Board that the license is active, unrestricted, and has no pending disciplinary actions. Specialty Certification: Confirming status with the American Academy of Family Physicians (AAFP) or the ABIM. Exclusion Checks: Running the provider’s name through the OIG (Office of Inspector General) and SAM (System for Award Management) databases to ensure they are not debarred from federal programs. The high cost of delays in this phase cannot be overstated. If a verification clerk at a residency program is on vacation, your enrollment file sits idle. Veracity recommends proactive follow-up every 48 hours until verification is received. Specialty-Specific Nuances: Family vs. Internal Medicine While both are primary care, the enrollment nuances between Family Medicine and Internal Medicine can impact how your contracts are structured. For Family Medicine providers, there is a heavy emphasis on procedural versatility. Payers may require specific proof of competency for in-office procedures like skin biopsies, joint injections, or IUD placements. If these are not properly documented during enrollment, the provider may be restricted from billing those specific CPT codes. You can learn more about these requirements in our specific guide to Family Medicine enrollment. Internal Medicine providers, conversely, often deal with more complex chronic care management. In 2026, payers are looking for “Value-Based Care” readiness. When enrolling these providers, it is essential to highlight any certifications in geriatric care or complex disease management. Our Internal Medicine enrollment guide provides a step-by-step breakdown of how to position these providers for maximum reimbursement tiers. Critical Billing Codes to Monitor 99202–99215: Standard E/M codes for office visits. G2211: The 2024+ add-on code for longitudinal care (essential for primary care). 99490: Chronic Care Management (CCM) services. 99487: Complex CCM services. Ensuring these codes are linked to the provider’s NPI and approved within the payer’s system is the difference between a profitable month and a revenue shortfall. The 2026 Strategy: Parallel Processing Waiting for one step to finish before starting the next is a relic of the past. To reduce the 120-day timeline by as much as 45 days, The Veracity Group implements a parallel processing model. As soon as the Primary Source Verification is underway, you should initiate the enrollment applications with individual payers like Blue Cross Blue Shield, Aetna, and UnitedHealthcare. By the time the internal committee grants approval, the payer applications should already be in the “review” phase of their queue. This proactive approach ensures that the provider is ready to see patients and: crucially: generate billable revenue the moment they walk through the
How to Credential Psychology Providers in 2026

In 2026, the demand for mental health services has reached an all-time high, making behavioral health provider enrollment the primary engine of your practice’s financial health. For psychologists, the path to a sustainable revenue stream is no longer a simple administrative task; it is a complex, high-stakes process that requires surgical precision. Whether you are a solo practitioner or managing a large multi-specialty group, understanding the intricacies of the 2026 landscape is the backbone of professional credibility. The landscape has shifted. Payers are more stringent, directories are under intense scrutiny due to “ghost network” regulations, and the federal government has streamlined yet tightened the requirements for Medicare and Medicaid enrollment for behavioral health providers. If your enrollment isn’t handled with expertise, your practice will face denied claims, out-of-network status, and significant revenue leakage. The Essential Documentation Framework Before you even log into a portal, you must have your professional house in order. Missing a single date or having a one-month gap in your CV can stall your application for months. In the psychology field, documentation is the silent driver of your success. You must compile: Current Professional CV: This must be in a month/year format with no unexplained gaps. State Licensure: Ensure your licenses for every state in which you practice are active and without encumbrances. Educational Verification: Proof of your PhD or PsyD from an accredited institution. Malpractice Insurance: Typically, payers require a minimum of $1 million/$3 million in coverage. NPI (National Provider Identifier): Ensure your Type 1 (Individual) and Type 2 (Group) NPIs are correctly categorized. Board Certifications: While not always mandatory, they provide a competitive edge in tier-one network placements. Alt Text: Botanical illustration of a tidy credentialing workspace with CAQH and NPI paperwork, signaling accuracy and compliance. CAQH ProView: Your Professional Passport The Council for Affordable Quality Healthcare (CAQH) remains the gold standard for data collection in 2026. Think of your CAQH profile as your passport to success. Almost every commercial insurance carrier, from Aetna to Cigna, pulls data directly from this repository. To avoid the high cost of delays, you must ensure your CAQH profile is 100% complete before authorizing payers to view it. Errors in your taxonomy codes: such as listing yourself as a general psychologist when you specialize in neuropsychology: will cause a mismatch in payer systems. This mismatch is a primary reason why behavioral health provider enrollment is so hard for those who attempt it without expert guidance. Furthermore, you must re-attest every 120 days. Failure to do so results in your profile becoming “inactive,” which triggers an automatic suspension of your provider status with many insurers. At The Veracity Group, we see this “set it and forget it” mentality ruin practice cash flows every single month. Navigating Medicare and Medicaid Enrollment for Behavioral Health Providers The 2026 federal requirements have integrated more psychology-specific qualifiers than ever before. For psychologists, enrolling in Medicare is no longer optional if you want to capture the aging demographic. The process involves the PECOS (Provider Enrollment, Chain, and Ownership System). When handling Medicare and Medicaid enrollment for behavioral health providers, you must be aware of the “Opt-Out” status. If you have previously opted out of Medicare, there is a specific timeline and process to opt back in. Medicaid enrollment is even more fragmented, as each state maintains its own rules. If you are operating across state lines: perhaps via PSYPACT: you must ensure your Medicaid enrollment is synchronized across all relevant jurisdictions. This is especially true for those following a behavioral health provider enrollment beginner’s guide who may not realize the complexity of multi-state compliance. The American Psychological Association (APA) provides updated guidelines on how these federal programs impact clinical practice, emphasizing the need for rigorous adherence to the latest billing standards. PSYPACT and Multi-State Authority In 2026, the Psychology Interjurisdictional Compact (PSYPACT) is the standard for tele-psychology. However, having PSYPACT authority does not mean you are automatically enrolled with insurance carriers in every compact state. You must still go through the enrollment process for each state’s specific network. The Association of State and Provincial Psychology Boards (ASPPB) oversees the E.Passport and IPC requirements. You must ensure these credentials are uploaded to your CAQH profile and individual payer applications. Without this, your tele-health claims for out-of-state patients will be rejected as “provider not found.” Alt Text: Botanical illustration of a telehealth-ready workspace showing secure network connectivity for psychology enrollment across states and payers. Specialty-Specific Coding and Taxonomy Precision in coding is what separates a thriving practice from one that is struggling. In psychology, your enrollment must reflect the specific CPT codes you intend to utilize. This includes: 90791: Psychiatric diagnostic evaluation. 90834 & 90837: Individual psychotherapy (45 and 60 minutes). 96130 & 96131: Psychological testing evaluation services. If your enrollment profile does not specifically authorize you for testing codes (96130 series), payers will deny these high-value claims regardless of your clinical expertise. You must ensure your taxonomy code (e.g., 103T00000X for Psychologists) is correctly mapped to your billing software and payer contracts. The High Cost of DIY Enrollment Many psychologists attempt to handle their own enrollment to save on upfront costs. This is often a serious consequence-laden mistake. The time you spend navigating the labyrinth of payer portals is time you are not spending with patients. At an average hourly rate for a psychologist, the opportunity cost of spending 20 hours on paperwork is thousands of dollars in lost clinical revenue. Moreover, the consequences of errors are permanent. A rejected application can lead to a “waiting period” where you are barred from re-applying for six months to a year. This gap can make or break a new practice. The Veracity Group provides the expert shield you need to avoid these pitfalls, ensuring your applications are processed correctly the first time. Payer-Specific Nuances: What to Watch For In 2026, payers have distinct “personalities” in their enrollment departments: UnitedHealthcare/Optum: Heavily relies on digital attestation and often requires specific “Clinical Specialty” forms for psychologists. Blue Cross Blue Shield:
How to Credential Radiology Providers in 2026
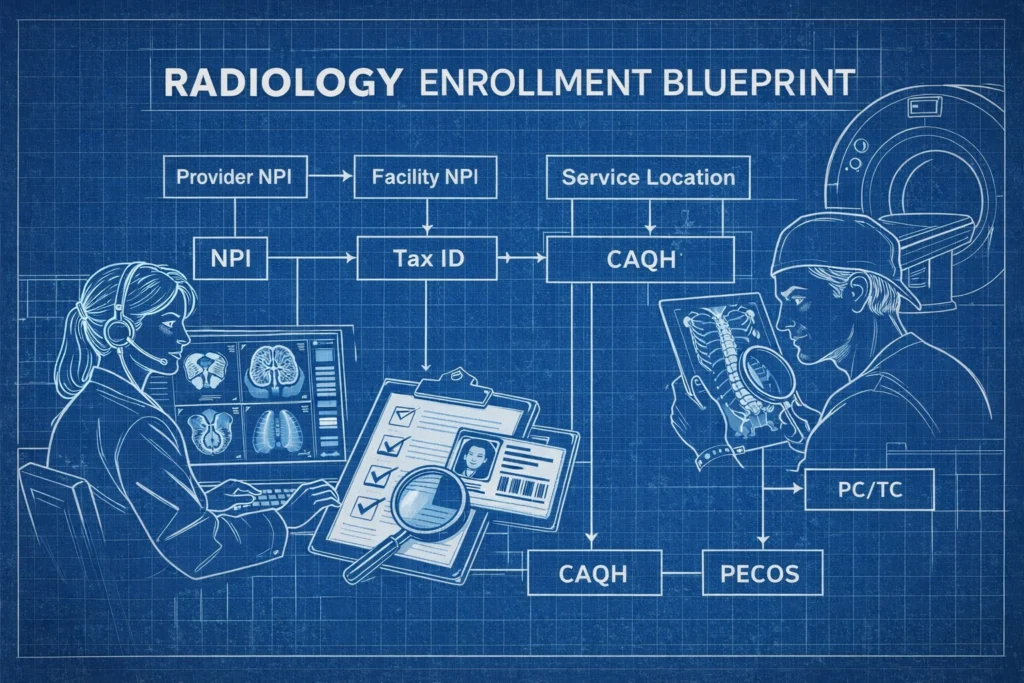
In the high-velocity world of diagnostic imaging, the efficiency of your medical provider enrollment services is the heartbeat of your practice’s financial health. As we navigate through 2026, the complexity of Radiology credentialing 2026 has intensified, driven by stricter federal regulations, the integration of advanced artificial intelligence in diagnostics, and a heightened focus on real-time data accuracy. For a radiology group or an imaging center, a single missing document or a delayed verification can halt revenue for months. The Veracity Group understands that in radiology, time is not just money: it is patient care. When a sub-specialized interventional radiologist cannot bill for a complex procedure due to a pending enrollment file, the entire facility feels the impact. This guide provides the definitive blueprint for navigating the current landscape with precision and authority. The Critical Nature of Radiology Enrollment in 2026 Radiology is a unique beast in the healthcare ecosystem. Unlike many specialties that focus on a single type of patient interaction, radiologists often work across multiple facilities, read for various medical groups, and utilize a wide array of high-tech modalities. This interconnectedness makes the enrollment process particularly volatile. In 2026, payers have moved toward continuous monitoring models. Gone are the days when you could submit an application and forget about it for three years. Today, licensing boards, the Office of Inspector General (OIG), and the National Practitioner Data Bank (NPDB) are under constant surveillance by automated payer systems. If your provider’s data is not perfectly synchronized across all platforms, your claims will be rejected instantly. Why Speed is Mandatory The standard window for completing the full enrollment cycle has tightened. While the industry average used to hover around 180 days, current expectations for accredited organizations have shifted toward a 90 to 120-day window. If your practice fails to meet these timelines, you face the high cost of “dark days”: periods where your highly-compensated radiologists are seeing patients but generating zero collectible revenue. Stage 1: Document Aggregation and ABR Certification The foundation of every successful enrollment file begins with the American Board of Radiology (ABR). In 2026, payers require instantaneous verification of board eligibility or certification status. You must ensure that every radiologist in your group has an updated, gap-free profile within the ABR database. Alt Tag: Blueprint / technical drawing MRI suite with labeled callouts supporting structured radiology provider enrollment documentation. Your documentation checklist must be exhaustive. Any “gap” in a provider’s timeline: even a two-month break between residency and a fellowship: is a red flag for modern auditors. You must secure: Current State Medical Licenses: All active licenses must be primary-source verified. ABR Certification Status: Documentation of Maintenance of Certification (MOC) is now a standard requirement for most commercial payers. Visit the ABR to verify current standards. Malpractice History: A full five-year claims history with no unexplained periods of non-coverage. Specialty Training: Specific documentation for sub-specialties such as Neuroradiology, Pediatric Radiology, or Interventional Radiology. For practices looking to streamline these initial steps, leveraging professional provider enrollment services is the only way to ensure that nothing slips through the cracks. Stage 2: Managing Professional and Technical Component Billing One of the most significant hurdles in Radiology credentialing 2026 is the management of the Professional Component (PC) and the Technical Component (TC). Radiologists frequently bill for the interpretation of an image (Modifier 26), while the facility bills for the equipment and staff (Modifier TC). If your enrollment is not structured correctly, payers may recognize the provider but not the location, or vice versa. This is a common point of failure for new imaging centers. You must ensure that: The provider is correctly linked to the group’s Tax ID. The group is properly enrolled at the specific service location NPI. The payer has confirmed receipt of the linkage for both the professional and technical components. Failure to manage these linkages results in “denied for lack of provider enrollment” messages, which are notoriously difficult to overturn retroactively. This level of detail is similar to the complexities found in our guides for Cardiology and Oncology enrollment, where facility-based billing is equally rigorous. Stage 3: Primary Source Verification and ACR Standards The American College of Radiology (ACR) sets the gold standard for clinical practice and facility accreditation. Payers in 2026 often cross-reference a provider’s enrollment application with the facility’s ACR accreditation status. If a radiologist is performing high-end MRI or PET scans in a facility that has let its ACR accreditation lapse, the provider’s individual enrollment will not save the claim from being denied. Alt Tag: Blueprint diagnostic workstation schematic highlighting ACR standards and primary source verification for radiology enrollment. The Primary Source Verification (PSV) stage is where Veracity excels. We contact the original issuers of credentials: medical schools, residency programs, and licensing boards: using direct API integrations. This removes the manual “wait and see” approach that characterizes slower, outdated enrollment methods. In 2026, manual verification is a liability. You must utilize digital-first strategies to stay ahead. Stage 4: Navigating CAQH and PECOS for Radiologists For any radiologist, the CAQH ProView profile is the backbone of their professional credibility. In 2026, payers use CAQH as their primary data source for directory updates and re-credentialing cycles. An incomplete CAQH profile is the fastest way to get dropped from a payer network. The Medicare Hurdle (PECOS) Medicare enrollment via the Provider Enrollment, Chain, and Ownership System (PECOS) remains the most demanding aspect of the process. Radiologists must be enrolled with the correct “Provider Type” to ensure that 70000-series CPT codes (Radiology) are processed without intervention. If a provider is accidentally enrolled under a general practice type, specialized interventional procedures may be flagged as “out of scope” for that provider. To avoid these risks, your team should perform a deep dive into CAQH and Medicare enrollment to ensure all data points align with the ACR guidelines for practice parameters. Stage 5: Continuous Monitoring and Sanction Screening In 2026, the concept of “set it and forget it” is dead. The Veracity Group implements a strategy of continuous monitoring.
How to Credential Podiatry Providers in 2026

In the rapidly evolving healthcare landscape of 2026, the administrative burden of bringing a new Doctor of Podiatric Medicine (DPM) into your practice is heavier than ever. Precision is no longer just a surgical requirement; it is a regulatory one. For podiatry practices, the process of getting a provider ready to see patients and, more importantly, get paid for those visits is the backbone of professional credibility. The complexity of podiatry provider enrollment stems from the specialty’s unique overlap between primary care, surgery, and durable medical equipment (DME). Without a proactive strategy, your practice faces the high cost of delays, leading to empty schedules and mounting overhead. At The Veracity Group, we see firsthand how streamlined medical provider enrollment services act as a catalyst for practice growth, ensuring that your specialists are revenue-ready from day one. The Foundation of Podiatric Enrollment in 2026 The year 2026 has introduced tighter windows for documentation and a zero-tolerance policy for data discrepancies. Before a single application is submitted, you must treat the pre-enrollment phase as a high-stakes audit. The foundational elements are the silent drivers of a successful launch. Every DPM must have their administrative house in order. This includes: Tax ID and NPI Alignment: Ensure the IRS Tax ID is correctly linked to both Type 1 (Individual) and Type 2 (Organizational) NPIs. CPME-Approved Residency Verification: Payers now require exhaustive proof of completion of a three-year podiatric medicine and surgery residency (PMSR) accredited by the Council on Podiatric Medical Education. Malpractice Coverage: In 2026, many carriers require “tail” coverage or specific retroactive dates to be clearly articulated in the certificate of insurance (COI) before they will even initiate a file. Alt Tag: Pencil sketch technical drawing of foot anatomy with enrollment checklist annotations and compliance markers. Primary Source Verification: The 2026 Standards The National Committee for Quality Assurance (NCQA) has significantly compressed the timeline for primary source verification. Organizations are now operating on a 90-to-120-day window, down from the much more lenient periods of the past decade. If your practice is still relying on paper-heavy, manual processes, you are already behind. Verifying a podiatrist requires specific outreach to the American Board of Podiatric Medicine (ABPM). Maintaining active status with the ABPM is a non-negotiable requirement for the majority of commercial and government payers in 2026. This verification must come directly from the board; a copy of a certificate provided by the physician is insufficient. Similarly, membership and standing with the American Podiatric Medical Association (APMA) often serves as a secondary layer of professional validation that payers use to assess the provider’s commitment to the field’s current standards of care. Navigating the DMEPOS Enrollment Maze Unlike many other specialties, podiatrists are frequently high-volume prescribers and providers of orthotics, therapeutic shoes, and other medical devices. This necessitates a separate, rigorous enrollment process for Durable Medical Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS). In 2026, the National Provider Enrollment (NPE) East and West contractors have intensified their site visit requirements. If your podiatry clinic provides L-coded items (such as L3000 for custom orthotics), you must ensure your physical location meets the 36 DMEPOS supplier standards. Failure to pass a DME site inspection can stall your Medicare Part B enrollment entirely, creating a massive bottleneck in your revenue cycle. Leveraging professional medical provider enrollment services is the most effective way to ensure your facility and your providers meet these specialized criteria simultaneously. Surgery Center Integration and Compliance Many podiatrists split their time between a private clinic and an Ambulatory Surgery Center (ASC). This dual-environment practice adds a layer of complexity to the enrollment process. Each location must be correctly tied to the provider’s NPI and Tax ID within the payer’s system. If your DPM is performing complex reconstructions or wound debridement in a surgical setting, the risk of claim denials increases if the enrollment is not mirrored across both the group and the facility. For practices expanding their surgical footprint, understanding medical group enrollment for surgery centers is vital to avoid compliance pitfalls that could lead to clawbacks or excluded provider status. Much like the precision required in orthopedics provider enrollment, podiatric surgery demands meticulous attention to detail regarding hospital privileges and admitting arrangements. Alt Tag: Sketch architectural network diagram linking a clinic and ASC with payer and compliance linework. Continuous Monitoring: Beyond the Initial Application The “set it and forget it” mentality of 2020 is dead. In 2026, payers utilize real-time monitoring software to track state licensure, OIG exclusions, and SAM sanctions. A single expired license or a missed CAQH re-attestation can trigger an immediate “out-of-network” status, resulting in thousands of dollars in lost revenue before you even realize there is a problem. For podiatry, this means keeping a constant watch on: State Podiatry Board Renewals: Each state has varying scopes of practice; ensure the provider’s license accurately reflects their current surgical or ankle-scope certifications. CAQH ProView Profiles: These must be updated every 90 days without exception. For a deep dive into maintaining these digital identities, navigating the maze of CAQH is essential reading for practice managers. DEA and CDS Certifications: Even if your podiatrist limits their prescribing, payers require active, unencumbered controlled substance registrations for the specific state of practice. Billing Specifics and the Impact on Enrollment Your podiatry provider enrollment strategy must be informed by your billing department. Podiatry-specific CPT codes, such as 11721 (nail debridement) or 11042 (skin debridement), are under constant scrutiny by Medicare Administrative Contractors (MACs). If the provider is not correctly enrolled with the appropriate taxonomy codes, specifically 213E00000X for Podiatrist or 213ES0131X for Foot & Ankle Surgery, claims will be rejected at the clearinghouse level. Just as an internal medicine provider must be linked to the correct primary care incentives, a podiatrist must be correctly identified to trigger the specialty-specific fee schedules you have negotiated. Veracity ensures that these taxonomy codes are not just a footnote, but a primary focus of the enrollment submission. Alt Tag: Sketch-style foundational blocks with subtle healthcare admin verification symbols representing enrollment stability. Why

