How to Credential a Speech-Language Pathology Provider: Therapy Enrollment Success

Securing a seat at the payer table for a Speech-Language Pathologist (SLP) is a rigorous process that demands precision, clinical documentation, and strict adherence to federal guidelines. When you look at how to credential a speech-language pathology provider, you are not just filling out forms; you are building the financial bridge between life-changing therapy and sustainable practice revenue. In the specialized world of rehabilitative services, a single clerical error or a missed clinical fellowship date can block your ability to collect on claims. As a result, every step in this process matters. The path to successful enrollment runs through specific certifications and state-mandated milestones. Unlike general practitioners, SLPs move through a landscape where both professional associations and state regulatory boards scrutinize their clinical competency. At The Veracity Group, we see every week how the high cost of delays in this sector often comes from a lack of “provider-readiness” before the application ever reaches the payer’s desk. That lack of readiness turns into stalled revenue, frustrated staff, and avoidable rework. The Professional Foundation: ASHA CCC-SLP and State Licensure The primary pillar of SLP enrollment is the Certificate of Clinical Competence in Speech-Language Pathology (CCC-SLP), awarded by the American Association of Speech-Language-Hearing Association (ASHA). Some state Medicaid programs may allow “Clinical Fellows” (those in their post‑graduate supervised year) to enroll under specific modifiers. However, most commercial and federal payers still expect the CCC-SLP designation before they treat the provider as fully credentialed. State licensure nuances add another layer of complexity. For instance, in California, a provider must navigate two distinct pathways depending on the practice environment. A clinical SLP needs a license from the State Speech-Language Pathology and Audiology and Hearing Aid Dispensers Board, which requires 300 hours of supervised clinical practicum and a passing score of 162 on the Praxis exam. By contrast, if that same provider plans to work within the school system, they must secure a Speech-Language Pathology Services Credential through the Commission on Teacher Credentialing. Failure to match the specific license type to the provider’s intended place of service often leads to application rejection. Before you initiate any enrollment, confirm that the provider’s state license is active and shows no disciplinary actions. You can also verify the standing of various state boards through the American Association of Dental Boards (AADB) which offers a framework for multi‑disciplinary regulatory oversight. In practice, this early verification step prevents months of preventable delay. National Registries and the Digital Identity Every successful enrollment journey starts at the National Plan and Provider Enumeration System (NPPES). Obtaining a National Provider Identifier (NPI) is the first mandatory step. At this stage, you must register the SLP as an individual (Type 1 NPI) and select the correct taxonomy code for a Speech-Language Pathologist (235Z00000X). If you choose the wrong taxonomy at the NPPES NPI Registry level, Medicare cross‑checks will fail later and trigger avoidable corrections. Once you secure the NPI, the CAQH ProView Portal becomes the backbone of the provider’s digital identity. Most major commercial payers, including Aetna, UnitedHealthcare, and Anthem, pull their primary source verification data directly from CAQH. Consequently, any gaps or outdated records inside CAQH ripple across every payer panel. Within CAQH, make sure you: Upload a current CV in month/year format. Provide a copy of the ASHA certification. Maintain updated malpractice insurance face sheets. In addition, you must attest to this data on a regular schedule. An expired attestation often becomes the silent driver of sudden network terminations and claim denials. In other words, CAQH is not a one‑time setup; it is an ongoing maintenance obligation. Medicare Part B Enrollment: Private Practice vs. Facility-Based Navigating Medicare (CMS) enrollment for an SLP requires a working knowledge of the CMS‑855I and CMS‑855R forms. The rules shift depending on whether the provider practices in a private setting or a facility‑based environment. Because of that, you cannot treat all SLP enrollments as interchangeable. For private practice SLPs, Medicare Part B enrollment offers the only path to bill for services directly. These providers fall under the “Physicians and Non‑Physician Practitioners” category for billing purposes. You must confirm that the practice location qualifies as a valid, CMS‑approved site and that the tax ID, NPI, and address data match across all systems. Otherwise, you invite development requests and payment holds. Facility‑based SLPs, such as those working in hospitals or Skilled Nursing Facilities, usually have their services bundled into the facility’s Part A billing or specific Part B outpatient schedules. In these cases, the SLP still needs enrollment to “order and refer” or to reassign benefits to the facility’s tax ID. However, they do not bill independently under their own Part B profile. This distinction shapes how you complete the CMS‑855I and CMS‑855R forms and how you track revenue downstream. Just as we discussed in our guide on how to credential an infectious disease provider, the integration of clinical data into the PECOS system is a high‑stakes step. If a provider’s PECOS record does not align with their Social Security records or ASHA profile, Medicare will issue a development request and pause the file. That pause can add months to your timeline and stall every claim tied to that provider. The Complexity of Coding and Reimbursement Standards While many medical specialties rely on a broad range of diagnostic codes, SLPs depend heavily on specific CPT codes for evaluation and treatment. Common examples include 92507 (treatment of speech, language, voice, communication, and/or auditory processing disorder) and 92523 (evaluation of speech sound production). These codes drive both authorization and payment, so accuracy here is non‑negotiable. SLPs do not use dental‑specific codes. Even so, the American Dental Association (ADA) CDT Codes illustrate the level of standardized coding rigor that all healthcare providers must respect. For SLPs, this mindset translates into close monitoring of the former “Therapy Cap,” now managed through the KX modifier threshold. You must link the provider’s enrollment to a practice that understands the Medicare Physician Fee Schedule (MPFS). Otherwise, the team may deliver services that look appropriate clinically but still end up denied
How to Credential an Infectious Disease Provider: Navigating Payer Policies

Managing an Infectious Disease (ID) practice requires more than clinical expertise; it demands a rigorous administrative backbone to ensure every physician is properly enrolled with payers. When you look at how to credential an infectious disease provider, you are looking at one of the most complex subspecialties in the internal medicine umbrella. Because ID specialists often split their time between inpatient consultations, outpatient clinics, and specialized programs like Ryan White clinics, a "one-size-fits-all" enrollment strategy will lead to immediate claim denials and significant revenue leakage. At The Veracity Group, we see practices struggle when they treat ID enrollment as a generic task. The reality is that ID providers have specific board certification requirements and federal program enrollments that do not apply to general practitioners. If you miss these nuances, your providers will be providing life-saving care that your practice simply cannot bill for. The Foundation: ABIM Certification and Specialized Training The first hurdle in understanding how to credential an infectious disease provider is the verification of their advanced training. Payers do not just look for a standard medical license; they require proof of subspecialty expertise. To be recognized as an ID specialist by major payers like Blue Cross Blue Shield, Aetna, and UnitedHealthcare, the provider must hold certification from the American Board of Internal Medicine (ABIM). This process confirms that the physician has completed a three-year Internal Medicine residency followed by a multi-year Infectious Disease fellowship. During the enrollment process, you must provide the primary source verification of these certificates. Failure to present active ABIM Infectious Disease certification often results in the provider being "down-coded" or enrolled only as a General Internal Medicine physician. This is a disaster for your reimbursement rates, as ID-specific consultation codes (like those used for complex sepsis management or multi-drug resistant organism treatment) may be rejected if the payer's system does not recognize the provider as a specialist. Alt Tag: A professional medical board certificate representing ABIM Infectious Disease certification for provider enrollment. Site of Service: Clinic-Based vs. Hospital-Based Enrollment A critical fork in the road for ID enrollment is the site of service. Most ID providers are "hybrid" providers, but payers require a primary designation that dictates how they are linked to your Tax ID. 1. Hospital-Based Enrollment If your provider primarily performs inpatient consultations, they must be enrolled with a hospital-basis designation. This involves ensuring that their National Provider Identifier (NPI) is correctly linked to the hospital’s facility credentials for Part B billing. Without this link, the "Inpatient Consultation" codes (99251-99255) will face immediate scrutiny. 2. Clinic-Based Enrollment For ID specialists operating an outpatient clinic: handling long-term antibiotic therapy or wound care: the enrollment must reflect the clinic as the primary practice location. This requires a full CAQH ProView profile update that lists the clinic’s demographics, office hours, and accessibility. At Veracity, we emphasize that you must synchronize these locations. If a provider is enrolled only at the hospital but bills for a clinic visit, the claim will be denied for "location mismatch." This is a common pitfall we address when managing our services for multi-location groups. The Ryan White HIV/AIDS Program Enrollment Perhaps the most unique aspect of how to credential an infectious disease provider is the integration with the Ryan White HIV/AIDS Program. If your practice receives federal funding to treat low-income or uninsured patients with HIV, the enrollment process enters a new level of complexity. Providers working within Ryan White-funded clinics must be specifically registered within the HRSA (Health Resources and Services Administration) databases. This is not a standard "payer" enrollment, but it is a prerequisite for your practice to receive the grant-based reimbursements associated with this specialized care. You must ensure the provider’s NPI is associated with the specific Grantee ID of your facility. Missing this step means your practice absorbs the high cost of antiretroviral therapies and intensive case management without the federal backstop designed to cover these expenses. Much like the complexities we've discussed regarding how to credential a pulmonology provider, ID requires a deep dive into program-specific regulations that generalists never encounter. Navigating the CAQH and PECOS Gauntlet The Infectious Diseases Society of America (IDSA) recommends that practices maintain meticulous records of a provider’s "attestation" history. For ID providers, the CAQH profile must be a living document. When you are determining how to credential an infectious disease provider, you must verify that the CAQH profile includes: Malpractice Claims History: ID is a high-risk specialty; payers will scrutinize any history of claims related to hospital-acquired infections or surgical site complications. Drug Enforcement Administration (DEA) Registration: Ensure the DEA address matches the primary practice site to avoid delays in prescribing controlled substances for pain management in chronic infection cases. Work History: Any gaps longer than 30 days must be explained in writing, or the application will be kicked back. For Medicare enrollment via the PECOS system, the provider must be listed under the specific specialty code for Infectious Disease (Specialty Code 44). If they are mistakenly enrolled under Internal Medicine (Specialty Code 11), you will lose the ability to bill at the specialist rate for complex cases. Alt Tag: A healthcare administrator meticulously updating a provider's PECOS and CAQH profiles on a laptop. The High Cost of Enrollment Delays In the world of Infectious Disease, timing is everything: both clinically and financially. The average enrollment cycle takes 90 to 120 days. If you wait until a provider’s start date to begin the process, you are looking at four months of "non-billable" time. Consider a scenario where an ID specialist sees 15 patients a day, with an average reimbursement of $150 per visit. A 90-day delay in enrollment represents a $202,500 loss in gross revenue. This is the "silent driver" of practice insolvency. You cannot afford to treat enrollment as an afterthought. You must be proactive, starting the process the moment the employment contract is signed. Strategic Maintenance and Revalidation Enrollment is not a "set it and forget it" task. Payers require revalidation every three to five years.
How to Credential a Pulmonology Provider: Payer Requirements and Critical Care Nuances

In the high-stakes world of specialized medicine, pulmonology stands as one of the most administratively complex fields for provider enrollment. When you are bringing a new pulmonologist into your practice, you aren't just filing paperwork; you are navigating a minefield of board certifications, overlapping sub-specialties, and diagnostic testing requirements that can stall your revenue cycle for months. Understanding how to credential a pulmonology provider requires more than a basic knowledge of NPIs and state licenses. It demands a surgical precision in handling the nuances of the American Board of Internal Medicine (ABIM) standards and the specific billing requirements for Pulmonary Function Testing (PFT). If your enrollment strategy is generic, your denials will be specific: and expensive. The Foundation: ABIM Pulmonary Disease Certification The first hurdle in the journey of how to credential a pulmonology provider is the validation of their ABIM Pulmonary Disease certification. Unlike general internal medicine, payers look for this specific sub-specialty designation to authorize the high-level E/M codes and specialized procedures common in respiratory care. To maintain a "participating" status with major payers like UnitedHealthcare or Aetna, the provider must demonstrate they have completed an ACGME-accredited fellowship. The American Board of Internal Medicine (ABIM) is the primary source for this verification. You must ensure that the provider's certification is not only active but that their Maintenance of Certification (MOC) status is up to date. Payers are increasingly auditing MOC status during the re-enrollment cycle, and a "Not Meeting MOC Requirements" status can lead to an immediate suspension of payment for pulmonary-specific CPT codes. The Pulmonology vs. Critical Care Enrollment Paradox A common pitfall when learning how to credential a pulmonology provider is the failure to distinguish between Pulmonary Disease and Critical Care Medicine. While many providers are dual-certified, payers often require separate enrollment tracks depending on where the services are rendered. Office-Based Pulmonology: Focuses on chronic condition management (Asthma, COPD, Interstitial Lung Disease). This requires standard professional enrollment linked to your clinic’s tax ID. Inpatient Critical Care: If your provider is covering the ICU, the enrollment must include the specific hospital locations and often involves a different set of taxonomies. If you fail to list the correct taxonomy code: such as 207RP1001X for Pulmonary Disease or 207RC0200X for Critical Care: claims for life-saving interventions in the ICU may be rejected as "service not consistent with provider specialty." The Veracity Group has seen numerous practices lose six-figure sums because they incorrectly bundled these two distinct disciplines under a single generic internal medicine taxonomy. Diagnostic Credentialing: The PFT Hurdle Pulmonology is heavily reliant on diagnostic testing, specifically Pulmonary Function Tests (PFTs). To bill for the technical component of these tests (the equipment and staff time), your practice must be credentialed as a diagnostic facility or have the provider’s enrollment specifically include the "Technical Component" (TC) of these procedures. Payers like Medicare have strict rules regarding the Primary Source Verification of the equipment used and the certifications of the technicians performing the tests. When you are looking at how to credential a pulmonology provider, you must also look at the diagnostic side: Are you billing for CPT 94010 (Spirometry)? Does the provider have the requisite "Professional Component" (PC) enrollment to interpret these results across state lines if using telehealth? Failure to align the provider’s enrollment with the specific PFT diagnostic codes used in your office will lead to the "silent driver" of revenue loss: the partial denial where the office visit is paid, but the diagnostic tests: the backbone of your profitability: are rejected. Essential Registries and Verification Sources To successfully navigate how to credential a pulmonology provider, you must utilize the industry-standard registries with 100% accuracy. Any discrepancy between these databases will trigger a manual review, adding weeks to your timeline. NPPES NPI Registry: This is where your taxonomy selection begins. Ensure the Pulmonology sub-specialty is the primary taxonomy. CAQH ProView Portal: This is the central "passport" for your provider. It must be updated every 90 days. For pulmonologists, ensure that hospital affiliations are meticulously documented. American Association of Dental Boards (AADB): While primarily for dental oversight, maintaining a pulse on all state licensing board standards is a part of our comprehensive compliance check to ensure no cross-specialty red flags exist. American Dental Association (ADA) CDT Codes: In cases where pulmonologists treat sleep apnea in conjunction with dental sleep medicine providers, understanding the interplay of CDT and CPT codes is vital for integrated care models. Strategic Integration with Sleep Medicine Often, pulmonology providers are also the lead clinicians for Sleep Medicine programs. If your provider is reading sleep studies or managing CPAP/BiPAP compliance, their enrollment must reflect this. There is a significant overlap here, and managing the dual-enrollment process is a specialty in itself. You can learn more about the complexities of related specialties in our guide on why behavioral health and specialized sleep enrollment is so difficult. Integrating these services requires a deep dive into the American Thoracic Society (ATS) guidelines, which many payers use as a benchmark for clinical necessity and provider qualification. The Consequences of Enrollment Delays When you don't act quickly to secure the enrollment of a pulmonology provider, the consequences are immediate. Pulmonologists often manage a high volume of high-risk patients. A delay in enrollment means: Patient Access Issues: Patients with urgent respiratory needs cannot be seen if the provider is "out of network." Uncompensated Care: Your practice will be forced to choose between turning patients away or providing care that will never be reimbursed. Administrative Burnout: Your billing team will spend hundreds of hours chasing "pending" statuses. At The Veracity Group, we specialize in the "backbone of professional credibility." We ensure that from the moment a pulmonologist signs their contract, the wheels are in motion to get them fully loaded into payer systems. Our comprehensive enrollment services are designed to handle the critical care nuances that generic billing companies simply don't understand. Summary Checklist for Pulmonology Enrollment To ensure you stay on track, follow this rigorous process for every new hire: Verify
How to Credential a Sleep Medicine Provider: A Clinical Guide to Payer Enrollment

The landscape of Sleep Medicine is a complex intersection of multi-disciplinary expertise and rigorous facility standards. For practice managers and healthcare executives, the process of bringing a new sleep specialist into a network is not a routine administrative task; it is a high-stakes clinical and financial necessity. When you fail to navigate the specific nuances of this specialty, you risk months of denied claims and a complete halt to your sleep lab’s revenue cycle. Understanding how to credential a sleep medicine provider requires more than a basic knowledge of NPI numbers and CAQH profiles. Because sleep medicine providers often transition from different primary boards: such as Internal Medicine, Psychiatry, or Neurology: the documentation requirements are uniquely stratified. If your enrollment strategy does not account for these specific pathways, your provider will remain “out of network” long after they have started seeing patients. The Multi-Disciplinary Credentialing Landscape Sleep medicine is unique because it is not a standalone residency. Instead, it is a sub-specialty that requires a foundation in another medical field. Payers are hyper-vigilant about verifying the underlying board certification before they will even consider the sleep medicine designation. The Dual Board Paths To successfully enroll a provider, you must provide proof of a valid certificate from a member board of the American Board of Medical Specialties (ABMS). Most sleep specialists follow one of three primary tracks: Internal Medicine: These providers must maintain their ABIM certification while demonstrating the completion of a formal sleep fellowship. Psychiatry and Neurology: Providers coming from this background must show a valid ABPN certificate. Family Medicine: While less common, these providers must complete at least 12 months of ACGME-accredited fellowship training. You must ensure that the provider’s American Board of Sleep Medicine (ABSM) certification is active and correctly mapped to their primary specialty in the payer’s database. A mismatch here is the silent driver of thousands of dollars in “provider not found” denials. The Facility Hurdle: AASM Accreditation Requirements One of the most significant roadblocks in learning how to credential a sleep medicine provider is the inextricable link between the physician and the facility. Unlike a general practitioner who can be credentialed to any office, most major payers (including Medicare and large commercial carriers like Aetna and UnitedHealthcare) require the facility itself to be accredited for the provider to bill for technical components of sleep studies. The American Academy of Sleep Medicine (AASM) sets the gold standard for these facilities. To bill for CPT codes like 95810 (Polysomnography) or 95811 (Polysomnography with CPAP), the facility must often prove it meets AASM standards for inpatient or outpatient care. The Veracity Take: If your provider is ready to work but your sleep lab’s accreditation has lapsed, you cannot bill for the services they perform. You must manage facility accreditation and provider enrollment as parallel, interdependent tracks. Similar to the rigorous requirements found when you credential an allergy provider, the documentation must be airtight and specialty-specific. Strategic Steps: How to Credential a Sleep Medicine Provider To avoid the high cost of delays, you must follow a disciplined, consequence-driven roadmap. Every day your provider is not correctly enrolled is a day of lost revenue that you can never recover. 1. Verify the Primary and Sub-Specialty Boards Before submitting a single application, confirm the provider holds an active board certification in sleep medicine from the ABSM or a relevant ABMS member board. If the provider is “Board Eligible” but not yet “Board Certified,” many payers will either reject the application or place them in a lower-tier reimbursement bracket. 2. Standardize the CAQH Profile The CAQH ProView portal is the backbone of professional credibility in the enrollment world. For a sleep medicine provider, you must: Upload the fellowship completion certificate. List the sleep medicine board certification under the “Specialty” section. Ensure the work history explicitly includes time spent in sleep labs or accredited centers. 3. Address the Medical Director Requirements If the provider will serve as the Medical Director of your sleep facility, you must submit additional documentation. AASM-accredited facilities require the Medical Director to participate in at least 10 AMA PRA Category 1 CME credits per year in sleep medicine. Payers often request proof of these credits during the initial enrollment or during periodic audits. Billing and Coverage Codes: The Sleep Medicine Specifics Credentialing is the passport to success, but your enrollment must be structured to allow for specific billing codes. If the payer does not recognize the provider as a specialist in sleep medicine, they will likely deny claims for advanced diagnostics. Key codes that require specific enrollment status include: 95800 & 95806: Home Sleep Apnea Testing (HSAT). 95807: Sleep study with recorded simultaneous ventilation and heart rate. 94660: CPAP management and initiation. Without the proper specialty designation in the payer’s system, these codes are frequently flagged as “not medically necessary” or “outside of provider’s scope of practice.” This is why a generic enrollment approach fails: you need a team that understands the full scope of professional services and how they relate to specific diagnostic tests. Consequences of Incomplete Enrollment The risks of an improper enrollment strategy are severe and immediate: Revenue Leakage: Claims for sleep studies are high-dollar items. A single week of denials can result in five-figure losses. Patient Frustration: When a patient is told their sleep study is not covered because the provider was not properly credentialed, your practice’s reputation takes a hit. Audit Vulnerability: If you bill for sleep studies without the required AASM accreditation or ABSM certification on file, you are a prime target for a retrospective audit. Payers will not hesitate to recoup payments made to “unqualified” providers. Navigating the 12-Month Compliance Window For new sleep labs, Medicare provides a specific timeline that you must follow to stay compliant. You must submit your credentialing application within 90 days of the organization’s deadline and achieve final status within 12 months. Failure to meet these windows will result in a forced cessation of all sleep-related billing. The process of how to credential a sleep medicine
How to Credential an Allergy Provider: Navigating Immunology and Payer Panels

The process of bringing a new specialist into your practice is the backbone of professional credibility and the primary driver of your revenue cycle. When you are looking at how to credential an allergy provider, the stakes are higher than in general medicine. Allergy and Immunology is a high-precision subspecialty that involves complex biologic therapies, long-term immunotherapy plans, and stringent board requirements. Failing to navigate these nuances correctly will lead to immediate claim denials and the exclusion of your providers from essential insurance networks. At The Veracity Group, we understand that specialized enrollment is not a “one size fits all” administrative task. It is a strategic necessity. If your provider is not correctly aligned with payer expectations regarding their specific training and board status, your practice remains at a standstill. The Foundation of ABAI Certification The primary authority for allergy and immunology in the United States is the American Board of Allergy and Immunology (ABAI). To successfully navigate how to credential an allergy provider, you must first verify that the candidate meets the rigorous ABAI standards. Unlike broader specialties, the ABAI requires a minimum of 24 consecutive months of full-time fellowship training in an ACGME-accredited allergy/immunology program. This fellowship is the “passport to success” for any provider seeking to join a commercial or government payer panel. Payers look for this specific designation to ensure the provider is qualified to manage complex allergic reactions and primary immunodeficiency diseases. You must ensure that the provider’s fellowship certificates and training logs are updated in the CAQH ProView portal before initiating any enrollment applications. Navigating the ABP and ABIM Pathways One of the most unique aspects of the allergy specialty is the dual-track entry system. Allergy providers do not come from a single residency background. They are typically board-certified in either the American Board of Internal Medicine (ABIM) or the American Board of Pediatrics (ABP) before they ever begin their immunology fellowship. Pediatric Allergy Specialists: Must maintain an active, unrestricted certification from the ABP. Adult Allergy Specialists: Must maintain an active, unrestricted certification from the ABIM. Dual-Certified Providers: Some providers hold both, allowing them to treat a lifespan of patients from infancy through geriatrics. When you are determining how to credential an allergy provider, you must verify which board they are affiliated with. Payers will cross-reference the provider’s primary board certification against their ABAI eligibility. If there is a lapse in the primary certification (ABP or ABIM), the ABAI certification: and subsequently their payer enrollment: is at significant risk. Specific Documentation for Allergy Enrollment The standard set of documents: NPI, DEA, and state license: is just the beginning. For an immunologist, payers require a deeper dive into their clinical history and peer standing. You must compile a comprehensive digital folder that includes: ABAI Diplomate Status: Proof of current certification or “Board Eligible” status. Keep in mind that “Board Eligible” status typically expires five years after fellowship completion. Recommendation Letters: Most top-tier payer panels and hospital systems require at least two letters of recommendation from ABAI-certified Diplomates or chiefs of medicine who can attest to the provider’s clinical competence in immunology. Malpractice History: A clean, 10-year claims history is essential. Because allergy specialists deal with high-risk interventions like venom immunotherapy and drug desensitization, any history of malpractice in these areas will trigger intense scrutiny during the enrollment process. DEA and CDS Certificates: Ensure the DEA address matches the primary practice location where the provider will be seeing patients. Discrepancies here are a leading cause of enrollment delays. If you find the complexity of these requirements overwhelming, our team at The Veracity Group can streamline the process through our comprehensive provider enrollment services, ensuring every document is verified before submission to avoid the high cost of delays. Payer Panels and Immunotherapy Restrictions The financial health of an allergy practice depends heavily on the ability to bill for specific CPT codes related to testing and treatment. Codes such as 95004 (Percutaneous tests) and 95117 (Professional services for allergen immunotherapy) are frequently flagged by payers for manual review. When you are learning how to credential an allergy provider, you must recognize that payers often have specific policies regarding who can supervise these services. While some payers allow non-allergists to administer shots, they almost always require the primary prescribing provider to be a credentialed specialist. If your enrollment is not completed under the correct specialty taxonomy (207P00000X for Allergy & Immunology), the payer may downcode your claims or deny them entirely, viewing the services as “not medically necessary” or “outside the scope of the provider’s recognized specialty.” Furthermore, organizations like the American College of Allergy, Asthma & Immunology (ACAAI) provide clinical guidelines that payers often use as benchmarks for “reasonable and necessary” care. Ensuring your provider is active within the ACAAI can bolster their professional profile during the initial network adequacy reviews performed by insurance companies. Clinical Competency and Risk Management Enrollment is not just about paperwork; it is about proving a level of safety to the insurance carrier. Payers want to see that the provider is equipped to handle the inherent risks of the specialty. This includes: Anaphylaxis Management: Evidence of current ACLS (Advanced Cardiovascular Life Support) certification is often a mandatory attachment for allergy providers. Facility Standards: Payers may request an office site visit or a description of the facility to ensure that emergency equipment (epinephrine, oxygen, respiratory devices) is present where immunotherapy is administered. If your practice is expanding into other high-risk or highly regulated fields, such as behavioral health or addiction treatment, the enrollment hurdles can feel even more steep. We have seen similar challenges in other areas, as discussed in our guide on why specialized provider enrollment is so difficult, where the intersection of state law and payer policy creates a complex maze for administrators. State-Specific Supervision and Scope of Practice Each state has its own medical board regulations regarding who can perform allergy testing and who must be physically present during the administration of antigens. When you are looking at how to
Weekend Update: The 15-Day Rule & New State Laws You Can’t Ignore

March 2026 is delivering real, operationally relevant enrollment news—the kind that makes or breaks access and cash flow. If your providers are not enrolled and active, your practice does not get paid. Full stop. At The Veracity Group, we translate regulation into execution so you keep providers billable, audit-ready, and ready to scale across states and payers. 1) CMS 2026 Final Rule: The 15-Business-Day Medicare Enrollment Response (Rural) CMS is putting a hard operational expectation on the table: a 15-business-day response time tied to Medicare enrollment applications for rural healthcare access. This is not a “nice-to-have” process improvement—this is a new tempo for how fast underserved communities can add clinicians and reopen capacity. As summarized by Azalea Health’s overview of the CMS 2026 Final Rule, CMS connects faster action on enrollment files to improving rural access and reducing administrative drag in high-need areas. Source: Azalea Health — CMS Final Rule 2026 The pain point (what breaks when you move fast) A shorter clock does not lower standards. It raises the cost of errors: RTPs and development requests still stop the line when identities, locations, or signatures do not validate. Inconsistent practice addresses across PECOS fields create friction that burns days you no longer have. Missing attachments (licenses, supporting documentation, or ownership disclosures when applicable) convert “15 business days” into lost weeks. The Veracity Take: How you win under the 15-day standard Treat the 15-day rule like an express lane with strict baggage limits: only clean packets get through. Your playbook: Pre-validate the “identity triangle”: NPI, taxonomy, and state license must match everywhere (PECOS, payer file, and internal roster). Standardize location logic: service location, pay-to, and correspondence addresses must be intentionally consistent, not “close enough.” Control the handoffs: one owner for application build, one reviewer for QA, and one person for payer follow-up—no shared inbox chaos. Start enrollment at signature: the contract date is the starting gun. A delayed submission is guaranteed revenue drag. If you are tightening your process across multiple jurisdictions, the same discipline scales when you are mastering multi-state Medicaid provider enrollment as part of one pipeline that stays clean under pressure. 2) Oregon (March 2026): Centralized Credentialing Platform for Behavioral Health Oregon is attacking a bottleneck that directly impacts access: administrative friction that slows behavioral health onboarding and extends patient waitlists. The new March 2026 law streamlines the process using a centralized platform, aiming to reduce burnout for staff and speed time-to-care. As reported by Becker’s Behavioral Health, the law focuses on simplifying workflow for behavioral health workers through a central system. Source: Becker’s Behavioral Health — Oregon law streamlines credentialing The Veracity Take: Enrollment consequences you must plan for Centralization changes how fast data moves—and how fast it becomes your problem if it is wrong: Your behavioral health roster (LCSW, LPC/LMHC, LMFT, Psychologists, PMHNP) must stay continuously accurate to avoid processing stops. A centralized workflow exposes duplicates and inconsistencies immediately (names, licenses, supervision status, and locations). Faster intake means your team must respond faster to document requests, or you lose the time savings. If you support behavioral health lines, you protect throughput by operationalizing what makes these files different—high volume, many provider types, and strict documentation. Your team stays ahead by understanding why behavioral health provider enrollment is so hard and building a repeatable intake standard. 3) Washington (January 2026): Physician Application Questions Updated to Reduce Stigma Washington moved early in 2026 to reduce mental health stigma by overhauling physician credentialing questions—removing barriers that discourage clinicians from seeking care and staying in practice. As reported by Becker’s Behavioral Health, Washington updated the question set to reduce stigma for physicians. Source: Becker’s Behavioral Health — Washington overhauls questions The Veracity Take: What you do with this change You do not “set it and forget it.” You: Update internal enrollment intake forms so you are collecting the right information—no outdated prompts that create rework. Train your onboarding team to keep questions aligned with the current standard and avoid avoidable escalations. Document your process so your files stay audit-ready and consistent across locations. What You Must Do This Week (Non-Negotiables) Enrollment is the silent driver of revenue. When it stalls, everything stalls. Build a 15-day-ready Medicare packet checklist (and enforce it) for rural or underserved locations. Run a roster hygiene sweep: NPI, taxonomy, license numbers, and addresses must match source-of-truth systems. Put behavioral health providers on a tighter cadence: faster state workflows demand faster internal response times. Lock in a maintenance rhythm so changes do not turn into denials later. A strong baseline is routine demographic updates that prevent payer file drift. Conclusion: Speed Is Now a Requirement, Not a Goal The CMS 15-business-day standard, Oregon’s centralized platform, and Washington’s updated question set all point to the same operational reality: enrollment is accelerating—and the penalty for sloppy data is rising. You do not win by working harder. You win by working cleaner. If you want a partner that runs enrollment with operational rigor and clear communication, The Veracity Group keeps your providers moving from signed to active without losing weeks to avoidable errors. #ProviderEnrollment #MedicareEnrollment #CMSFinalRule #RuralHealth #HPSA #PECOS #ProviderOnboarding #EnrollmentCompliance #EnrollmentOperations #PayerEnrollment #MedicareProviderEnrollment #BehavioralHealth #PMHNP #LCSW #LMFT #PhysicianEnrollment #MultiStateEnrollment #MedicaidEnrollment #DemographicUpdates #RevenueCycle #ClaimDenials #AuditReady #PracticeOperations #HealthcareAdministration #TheVeracityGroup Disclaimer: This blog post is for informational purposes only and summarizes publicly reported policy updates. Examples are illustrative and not patient-specific case studies.
DEA, CSR, and State Licenses: The “Triple Threat” of Provider Onboarding

In the high-stakes environment of modern healthcare, the distance between hiring a top-tier provider and that provider actually seeing their first patient is often a bureaucratic chasm. This gap is defined by the "Triple Threat" of provider onboarding: State Medical Licensing, Controlled Substance Registration (CSR), and Federal DEA Registration. For healthcare administrators and practice owners, these three pillars represent the backbone of professional credibility and the absolute prerequisite for clinical operations. However, they are not merely items on a checklist; they are a complex, sequential puzzle where a single missing document or a misread deadline acts as a silent driver of revenue loss. At The Veracity Group, we see the operational rigor required to navigate these waters every day. If your practice treats onboarding as an administrative afterthought, you are likely leaking thousands of dollars in potential revenue before your new hire even puts on a stethoscope. The Sequential Trap: Why Timing is Everything One of the most common mistakes in medical provider enrollment services is attempting to tackle these three requirements simultaneously. In the world of regulatory compliance, sequence is king. The State Medical License: This is the foundational requirement. You cannot apply for state-level prescribing authority or federal registration without an active, unrestricted license in the state where the provider will practice. State-Level Controlled Substance Registration (CSR): Approximately half of U.S. states require a secondary, state-specific permit to handle controlled substances. This must typically be secured after the medical license but before the federal DEA application. Federal DEA Registration: The final step. The DEA requires both the state license and (where applicable) the state CSR to be active before they will issue a federal registration number. If you attempt to jump to the DEA application without the prerequisite state CSR, your application will be rejected. This doesn't just result in a lost application fee; it resets the clock on the entire onboarding timeline, pushing back your "go-live" date by weeks or even months. The $1,550 Daily Leak: The Financial Reality of Delay The cost of licensing delays is not theoretical: it is a mathematical certainty that directly impacts your bottom line. Let’s look at the financial reality of a typical physician generating approximately $400,000 in annual net revenue. When you break that down into working days, that provider is responsible for roughly $1,550 in revenue per day. A 5-day delay (waiting for a transcript to be mailed): $7,750 lost. A 14-day delay (missing a CSR filing window): $21,700 lost. A 30-day delay (re-submitting a rejected DEA application): $46,500 lost. For a multi-provider group or a rapidly scaling telehealth platform, these numbers multiply exponentially. A delay in medical provider enrollment services isn't just an administrative headache; it is a massive financial hemorrhage. When your provider is ready to work but the paperwork is stuck in a state board’s fax machine, your practice is paying for overhead without the offsetting revenue. The Administrative Nightmare: Why It’s Harder Than It Looks On the surface, filling out a form seems simple. In practice, obtaining a state license is an exercise in forensic history. State boards often require 40-page applications that demand: Verified transcripts from medical schools attended decades ago. Letters of recommendation from residency directors who may have retired. Primary source verification of every hospital affiliation held in the last ten years. Strict adherence to "fax-only" communication from antiquated state coordinators. Managing this for one provider is a full-time job. Managing it for a dozen providers across multiple states: especially for telehealth practices expansion: is a logistical mountain. The Veracity Group’s 4-Step "Triple Threat" Solution The Veracity Group eliminates the guesswork and the "wait-and-see" approach to onboarding. We provide an end-to-end management system designed to navigate the specific nuances of all 50 states, the Interstate Medical Licensure Compact (IMLC), and the federal DEA Diversion Control Division requirements. Our process is built on operational rigor: 1. Intake & Assessment We don't just ask for a CV. We perform a deep dive into the provider’s history to identify potential red flags (gaps in work history, previous board actions, or expired registrations) that could trigger a board investigation or delay. 2. Document Coordination We act as the "boots on the ground," chasing down transcripts, verification letters, and peer references. We handle the "fax-machine loop" so your clinical staff doesn't have to. 3. Application & Submission We ensure every box is checked and every sequence is followed. We handle the state license first, the CSR second, and the DEA third, ensuring a seamless flow that satisfies the strict requirements of provider enrollment. 4. Board Follow-Up Submitting the application is only 50% of the work. The real battle is won in the follow-up. We maintain consistent communication with board analysts to ensure your application doesn't sit at the bottom of a digital pile. Scaling Across State Lines: Telehealth and Locums For groups expanding into "border markets" (such as a practice serving the NY/NJ/CT tri-state area) or national telehealth groups, the "Triple Threat" becomes even more dangerous. Each state has unique rules regarding CSRs and whether a provider needs a separate DEA number for each state where they prescribe. Failure to understand these nuances can lead to serious compliance risks. As of June 27, 2023, the DEA also requires a one-time 8-hour training requirement on the treatment and management of patients with opioid or other substance use disorders. Do your providers have their certificates ready? If not, their next DEA renewal will be blocked. Proactive Maintenance: The "Never-Lapse" Policy The most dangerous phone call a practice manager can receive is from a provider standing in front of a patient, unable to send a prescription because their DEA registration lapsed the night before. The Veracity Group provides proactive renewal management. We track expiration dates for licenses, CSRs, and DEA registrations months in advance, ensuring that renewals are filed and confirmed long before they reach the "red zone." This level of foresight is what separates a high-functioning practice from one that is constantly in crisis mode. Conclusion: Stop Chasing
Provider Enrollment in New York: PNDS + Dual Eligible Unwind
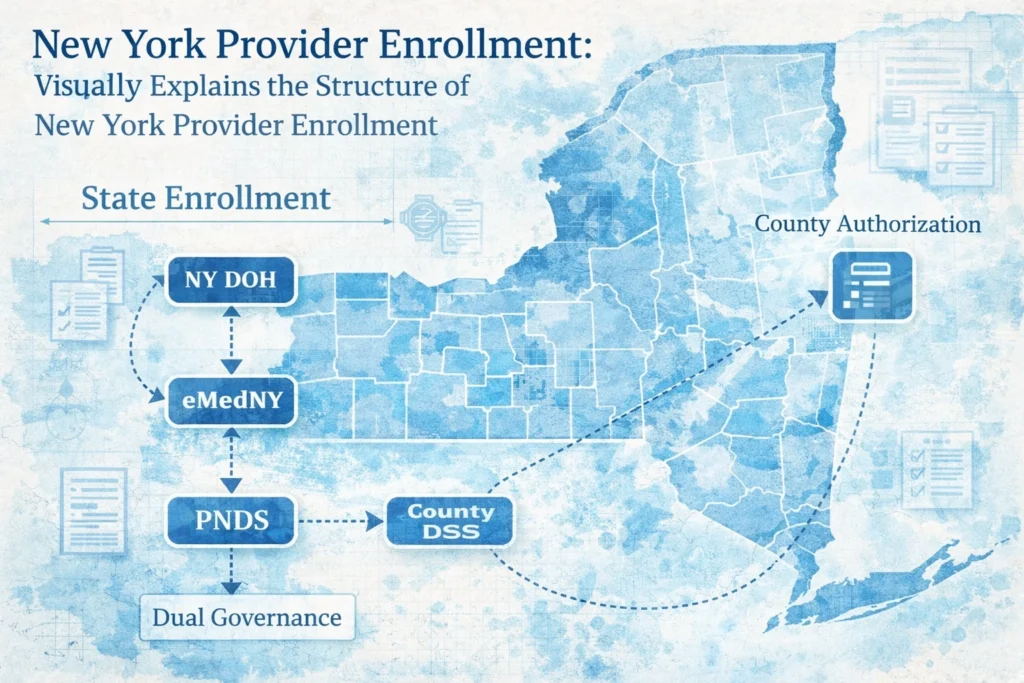
New York provider enrollment isn’t just complicated: it’s layered with administrative tripwires that derail even experienced practice managers. While most administrators focus on state-level Department of Health requirements, they miss how managed care network reporting, ongoing Provider Network Data System (PNDS) expectations, and NPI linking failures create a perfect storm of delays that cost your practice thousands in lost revenue. If you’re managing a multi-location clinic or expanding into New York for the first time, you’re walking into one of the most complex enrollment landscapes in the country. New York is uniquely challenging, but every state brings its own set of hurdles. See how it compares to other regions in our guide on Three States, Three Realities: Medicaid Enrollment in Texas, Indiana, and California. Here’s what most practice managers don’t know: and what will cost you if you don’t address it. 1) The Real New York Trap: Enrollment + Network Participation Drift New York Medicaid enrollment succeeds or fails based on clean, consistent provider data and plan-facing participation rules. Your eMedNY enrollment, your NPPES record, and the way Managed Care Organizations (MCOs) list you in their networks must align under the broader managed care oversight framework described on Medicaid.gov. This creates the operational trap: your practice can be enrolled but still not paid when your network participation data, provider directory listing, or plan configuration does not match what the MCO reports. What “Participation Drift” Looks Like in Real Life When your practice expands locations, adds providers, or changes tax details, you must keep every system synchronized. Drift shows up as: Rendering providers missing from a plan’s active roster even though your clinic treats members Incorrect service locations in plan directories that block referrals and generate grievances Tax ID / pay-to mismatches that trigger claim denials or payment holds Role configuration errors (billing vs. rendering vs. servicing) that reject claims at intake For high‑Medicaid specialties (behavioral health, pediatrics, family medicine, urgent care), these gaps create immediate revenue disruption because volume is high and denials compound fast. 2) eMedNY Enrollment vs. PNDS: Know What Each System Actually Does New York’s eMedNY remains the backbone of Medicaid claims processing and provider enrollment workflow. PNDS is different. PNDS is a managed care provider network reporting tool used for oversight of MCO networks—plans submit provider network data and the state evaluates network adequacy. New York DOH describes PNDS as a managed care provider network data system (see NYSDOH PNDS overview). In federal context, Medicaid managed care oversight relies on accurate network reporting as part of monitoring and access expectations (see Medicaid.gov managed care monitoring tools guidance). Why PNDS Accuracy Still Impacts Your Payments Because MCOs use provider network data to build rosters and directories, bad data turns into operational denial triggers. When your information is wrong in a plan’s network file, you see: Claims pended or denied due to provider/location not recognized for the member’s plan Referral leakage because patients can’t find you in directories Credentialing/contracting rework inside the plan (even when you already treat members) Network participation gaps that stall new site launches The Data Fields That Trip Up Most Practices During PNDS transition, these specific data elements cause the most enrollment failures: Service location addresses that don’t exactly match IRS tax documents Taxonomy codes that don’t align with actually rendered services Group NPI versus individual NPI designation errors Doing Business As (DBA) names that differ from legal entity names Supervising provider relationships for behavioral health services Even a minor discrepancy: like using “Street” instead of “St.” in your address: can trigger a validation failure that delays your enrollment by 45-60 days. NPI Linking: The Silent Enrollment Killer NPI linking failures represent the single most common reason for New York provider enrollment delays. The state requires precise relationships between individual provider NPIs, group NPIs, and service location NPIs: and if these relationships aren’t established correctly in both NPPES and eMedNY, your entire enrollment grinds to a halt. How NPI Linking Actually Works (And Where It Breaks) When you enroll in New York Medicaid, you must establish clear hierarchical relationships: Individual providers must be linked to the group NPI under which they practice Service locations must be associated with the correct group NPI Rendering providers must have active individual NPIs properly linked to billing entities Supervising providers must be explicitly linked to supervised staff for behavioral health services The problem? These relationships must be established in NPPES first, then replicated exactly in eMedNY, and now again in PNDS. Any mismatch creates a validation error that prevents enrollment completion. For practices offering medical provider enrollment services across multiple specialties, NPI linking becomes exponentially more complex. You’re managing multiple provider types, various supervision structures, and different taxonomy codes: all of which must align perfectly across three separate systems. The 30-Day NPPES Update Window Here’s a trap most practice managers fall into: they update NPI information in NPPES but immediately attempt to complete their eMedNY enrollment. NPPES changes take 7-10 business days to propagate to state Medicaid systems. If you submit your New York enrollment before NPPES updates are visible to eMedNY, your application will be rejected for data inconsistencies: even though your NPPES data is technically correct. You must wait for full NPPES propagation before proceeding with state enrollment. 4) The Real Consequences of eMedNY + Network Reporting Failures These aren’t theoretical problems: they create immediate revenue disruptions for practices that underestimate New York’s enrollment and managed care participation requirements: 1) Lost Revenue During Delays: Every week of enrollment delay costs practices an average of $8,000-$15,000 in unbillable Medicaid services, depending on patient volume. For behavioral health practices with high Medicaid patient populations, a 90-day delay means $50,000+ in lost revenue. 2) Directory and Roster Breakage: When your practice location, taxonomy, or provider affiliation is wrong in an MCO’s network data, patients search directories and never find you—even while your front desk schedules them. 3) Retroactive Billing Limits: New York allows limited retroactive billing (typically 60-90 days from enrollment approval), but services delivered during prolonged enrollment
Why Provider Enrollment Keeps Stalling: Q&A

Every practice eventually hits the same wall: “Why is this taking so long?” Most delays aren’t caused by payers being slow. Instead, they’re caused by missing data, misaligned records, or a breakdown between enrollment, contracting, and provider setup. This Q&A breaks down the real reasons applications stall and how to fix them. Q: Why does my provider enrollment keep getting stuck with no updates? A: Because payers rarely notify you when something is missing. If even one data point doesn’t match : NPI, CAQH, W‑9, taxonomy, address, or ownership : the application sits in limbo. Consequently, the payer won’t move it forward, but they also won’t tell you it’s stuck. You’re left in the dark while your revenue waits. Q: What is the #1 cause of enrollment delays? A: Data mismatch. If your NPI, CAQH, W‑9, and practice documents don’t match exactly, the payer cannot load your record. As a result, provider enrollment stops before any downstream steps begin (like credentialing or contracting). This is the single most preventable cause of delays. Nevertheless, it’s also the most common. Q: Why does the payer say they “never received” my provider enrollment application? A: They did receive it : but it failed an internal validation check. When that happens, the system rejects it before a human ever sees it. From your perspective, it looks like the payer lost it. In reality, the file never cleared the first gate. Automated rejection is silent. Therefore, your application appears to vanish into thin air. Q: Why does credentialing take so long when provider enrollment was submitted weeks ago? A: Because provider enrollment still isn’t complete. Credentialing only begins after provider enrollment is accepted. If enrollment is incomplete, credentialing never receives a clean file. You think you’re waiting on credentialing. In fact, you’re still waiting on provider enrollment to clear. For a plain-English breakdown of the difference, read: Enrollment vs. Credentialing. Q: What is the fastest way to prevent enrollment stalls? A: Clean data prevents stalls. Follow these steps: Keep CAQH ProView attested Match NPI and W‑9 addresses Use the correct taxonomy Link the provider to the group NPI Submit enrollment in the correct sequence Track each payer’s rules separately Clean provider enrollment = faster credentialing. When your data is consistent across every system, payers can process your application without friction. Otherwise, you’re creating your own delays. Q: Why do some providers get enrolled quickly while others take months? A: Because every provider has a different risk profile. Payers scrutinize: Work history gaps Malpractice claims Sanctions Multiple state licenses High‑risk specialties Two providers in the same practice can have completely different timelines. Moreover, your personal credentials determine your processing speed : not your practice’s reputation. Q: Why do claims reject even after the provider is “approved”? A: Because approval is not activation. Claims only pay after: Contracting is completed Payer setup is finalized The provider is loaded into the billing system Credentialing approval ≠ billable status. You can be credentialed and still unable to bill. Therefore, approval is only the midpoint : not the finish line. Q: Why do payers keep asking for the same documents repeatedly? A: Because each department operates independently. Provider enrollment, credentialing, contracting, and provider data management don’t share files internally. One department may have your documents : another may not. It’s inefficient, but it’s normal. Consequently, you’ll be asked for the same license or W-9 multiple times. Q: Why does my Medicaid enrollment take longer than commercial plans? A: Because Medicaid enrollment is state-governed. Your application runs through state-level verification and state-specific regulations, not a single national workflow. In practice, that means each state (and its Managed Care Organizations/MCOs) enforces its own layers of review, including: Ownership and controlling interest checks Site visits and location validation Background screening and exclusion checks State-specific forms, portal steps, and timelines MCO-specific roster, attestation, and document rules Medicaid is the slowest payer by design. When your state and its MCOs require multiple validation gates before they load you into their system, weeks turn into months—especially if one item fails validation and the file stalls without a clear notice. Q: Who can manage provider enrollment first, then coordinate the downstream steps? A: The Veracity Group. Veracity manages the entire lifecycle starting with provider enrollment (our specialty), plus coordination across downstream steps like credentialing, contracting, payer setup, and ongoing maintenance. As a result, each step moves cleanly into the next without stalls or mismatches. This eliminates the “handoff gaps” that cause most delays. Instead of juggling multiple departments and missing documents, you get a single, continuous process. The Bottom Line Most enrollment delays aren’t caused by payers. They’re caused by: Missing data Mismatched records Incorrect sequencing Poor follow‑up Disconnected workflows When provider enrollment, credentialing, contracting, and payer setup are managed as one continuous process, timelines shrink and revenue flows faster. Your provider enrollment isn’t stalled because payers are slow. It’s stalled because the system is broken : and no one is managing the handoffs. Veracity fixes the handoffs. Therefore, your providers get enrolled, then credentialed, contracted, and activated without the stalls, the silence, or the lost revenue. Ready to stop waiting and start billing? Contact The Veracity Group today to streamline your provider enrollment process and eliminate the delays that are costing your practice revenue. #ProviderEnrollment #PayerEnrollment #HealthcareBilling #RevenueCycleManagement #ProviderOnboarding #MedicaidEnrollment #ClaimsDenials #PracticeOperations #HealthcareCompliance #ProviderData #Credentialing #MedicalGroups #HealthcareAdmin #Clinics #MedicalStaffing #HealthIT #InsurancePaneling #PatientAccess #RevenueIntegrity #MedicalBilling #ProviderRelations #HealthcareManagement #PracticeManagement #Compliance #VeracityGroup
The Hidden Source of Most Provider Enrollment Delays: NPI & Payer Setup

Most provider enrollment delays don’t start with the payer. They start with the data behind the application : specifically your NPI, your provider setup, and your payer setup. These three elements form the backbone of every provider enrollment and credentialing workflow, yet they’re the most overlooked parts of the entire process. If you’ve ever wondered why your insurance provider enrollment stalls even when your documents are complete, the answer is almost always the same: the payer can’t load your record because the foundational data doesn’t match. Let’s break down why this happens and how to fix it. NPI Enrollment: The First Point of Failure Your NPI file is the source of truth for every payer.If your NPI enrollment contains outdated taxonomy codes, incorrect practice locations, or mismatched ownership details, every downstream process inherits the error. Payers cross‑check your NPI against: CAQH IRS records NPPES State licensure EFT/ERA documentation Group affiliations If anything is inconsistent, the payer pauses the application : often without telling you why. NPI issues don’t look like denials.They look like silence. Provider Setup: The Most Misunderstood Step in Provider Enrollment Most practices think “provider setup” is just entering a name and NPI into a system.It’s not.It’s the structural definition of how the provider exists inside your organization. A clean provider setup includes: Correct taxonomy Accurate specialties Linked service locations Proper group affiliations Matching practice structure across systems If your provider setup is wrong, payers can’t map the provider to the group.If they can’t map the provider, they can’t complete provider enrollment.If they can’t complete provider enrollment, they can’t load the provider into the network. This is why setup errors create long, quiet delays. Payer Setup: The Step That Determines Whether Claims Will Ever Pay Even when provider enrollment is approved, claims won’t pay unless the payer setup is correct.This is the part most practices discover too late : usually after the first batch of claims rejects. A clean payer setup ensures: The provider is linked to the correct group The taxonomy matches the NPI file The service locations are active The billing structure is recognized The provider is loaded into the payer’s directory If any of these elements are missing, the payer can’t activate the provider : even if provider enrollment is complete. This is why practices say, “We’re enrolled, but we still can’t bill.”Provider enrollment isn’t the finish line.Payer setup is. Why Insurance Provider Enrollment Depends on All Three Provider enrollment is the operational workflow that gets your provider and group loaded, linked, and active with each payer so you can bill without disruption. When your NPI enrollment, provider setup, and payer setup do not match, the payer cannot build or activate your record—and your revenue stalls. Payers rely on your NPI enrollment, provider setup, and payer setup to validate: Who you are Where you practice How you bill How you’re structured How you should be loaded into the network If any of these elements are misaligned, insurance provider enrollment stalls : not because the payer is slow, but because the data doesn’t support activation. Provider enrollment is an infrastructure process.If your setup is not clean, the payer cannot turn the lights on for billing. How to Fix Setup‑Driven Delays Before They Start 1. Audit Your NPI EnrollmentConfirm that taxonomy, addresses, and ownership details match your current structure in NPPES and across your internal systems so payer validation does not stall (NPPES). 2. Standardize Provider SetupCreate a template for every new provider so nothing is missed, and keep your identifiers current to prevent downstream mismatches. Use this quick, practical checklist to keep the basics clean: NPI Management. 3. Align Payer Setup With Your NPIIf the payer setup doesn’t match the NPI file, the application will stall. 4. Treat Setup as a Pre‑Provider Enrollment StepProvider enrollment should never begin until setup is complete. The Bottom Line Most provider enrollment delays aren’t payer delays at all.They’re setup delays. When your NPI enrollment, provider setup, and payer setup are aligned, provider enrollment becomes predictable. When they’re not, the process becomes a maze of silent stalls and unexplained slowdowns. Clean setup creates clean provider enrollment. This is exactly why demographic update delays are so costly: they break the very foundation your billing relies on. Clean provider enrollment creates clean billing.Clean billing creates clean revenue. That’s the operational chain ; and it always starts with setup. #Veracity #ProviderEnrollment #PayerEnrollment #NPIEnrollment #NPI #NPPES #ProviderOnboarding #PayerSetup #EnrollmentOperations #RevenueCycleManagement #ClaimsManagement #DenialPrevention #HealthcareCompliance #HealthcareOperations #PracticeManagement #MedicalGroupManagement #MultiStateEnrollment #ProviderDataManagement #HealthcareAdministration #MedicalBilling #EFTandERA #TaxonomyCodes #ProviderDirectory #CleanClaims #AuditReady

