The “Hidden” Cost of Enrollment Delays: Is Your Revenue in Payer Purgatory?

You’ve spent months recruiting the perfect specialist. The contract is signed, the lab coats are embroidered, and the patients are already calling to book appointments. But there is a silent predator lurking in your administrative hallway, ready to devour your projected quarterly earnings: the provider enrollment landscape. If your provider isn't fully linked to your payers, they aren't just "waiting to start": they are a massive financial liability. In the world of medical provider enrollment services, we call this "Payer Purgatory," a state where clinical work is performed, but the checks never arrive because of a single missing document, an expired license, or a CAQH mismatch. Looking for professional provider credentialing services in the USA? 👉 Check our main service page here: veracityeg.com The 180-Day Black Hole: Why Your Revenue is Ghosting You In an ideal world, you submit an application, and the payer moves it through the system with the speed and precision of a Swiss watch. In reality, the process is closer to tossing a message in a bottle into a stormy sea. Most practices find themselves trapped in a 90–180 day "black hole" of payer processing. During this window, your provider is effectively invisible to the insurance company’s payment system. The cost of this invisibility is staggering. Industry data suggests that enrollment delays can cost over $120,000 on average per provider. When you scale that across a multi-specialty group or a growing surgical center, you aren't just looking at a minor accounting hiccup; you’re looking at a structural threat to your practice’s survival. For specialists like surgeons or cardiologists, the stakes are even higher, with potential losses frequently exceeding $200,000 in stalled revenue for a single delayed enrollment. The Anatomy of a Delay: How One Paperclip Can Cost $100k Why does it take so long? The complexity of Medicare and Medicaid enrollment combined with the fractured requirements of private payers creates a minefield. A single "hidden" error is all it takes to trigger a rejection that sets you back to day one. Consider these common, yet devastating, "tiny" errors: CAQH Mismatches: If your CAQH profile lists a previous practice address but your new application lists the current one, the payer’s automated system will flag it as a discrepancy. Expired Supplemental Docs: A DEA certificate or state license that expires during the 120-day review period can bring the entire process to a screeching halt without the payer notifying you for weeks. Attestation Gaps: Forgetting to re-attest on CAQH every 90 days is the fastest way to turn a "pending" application into a "denied" one. According to the American Hospital Association, administrative complexities and payer delays are a primary driver of financial instability in healthcare. When these errors occur, the "dollars on hold" queries start spiking in your billing office, and by then, the damage is already done. The Back-of-the-Envelope Formula: Calculate Your Exposure Most administrators know they are losing money during delays, but few have quantified the exact "financial bleed." Understanding your exposure is the first step toward justifying a more robust approach to medical provider enrollment services. Use this simple formula to estimate how much revenue is currently sitting in Payer Purgatory for your practice: The Revenue Exposure Formula: Exposure = (Average Daily Revenue) x (Days in Enrollment Limbo) Let's look at two illustrative scenarios: The General Practitioner: If a primary care provider generates $1,200 in billable revenue per day and is stuck in a 120-day enrollment delay, your practice is sitting on $144,000 in uncollectible or delayed funds. The Specialist Surgeon: For a high-volume specialist generating $6,000 daily, a 150-day "black hole" results in a massive $900,000 revenue risk. Even if you eventually get paid through retroactive billing, the cash flow disruption can prevent you from meeting payroll, investing in new equipment, or expanding your medical group enrollment for surgery centers. The Myth of Retroactive Billing A common trap for practice managers is the "we’ll just bill it later" mentality. This is a dangerous gamble. While Medicare and Medicaid enrollment rules occasionally allow for limited retroactive billing (often capped at 30 days prior to the filing date), many private commercial payers offer zero leeway. If your provider sees a patient on Day 1, but the "Effective Date" granted by the payer is Day 60, those two months of clinical work are essentially donated services. You cannot bill the patient, and you cannot bill the payer. This revenue doesn't just arrive late; it vanishes entirely. Furthermore, even when retroactive billing is allowed, the administrative cost to resubmit hundreds of "held" claims is immense. Enrollment teams already spend upwards of 30+ hours per week simply tracking status updates across dozens of portals. Adding a massive backlog of claim re-submissions to that workload is a recipe for staff burnout and further demographic update errors. Beyond the Top Line: The Hidden Operational Drain The cost of enrollment delays isn't just found on the balance sheet; it’s found in the "soft costs" of operational inefficiency. Manual Tracking: If your staff is manually logging into 20 different payer portals to check status, they aren't focusing on patient care or revenue cycle optimization. Claim Denials: Research shows that roughly 15% of private payer claims are initially denied. A significant portion of these are tied directly to eligibility and enrollment inaccuracies. Patient Dissatisfaction: When a provider isn't "in-network" because of a paperwork delay, patients receive unexpected bills. This destroys the provider-patient relationship before it even begins. To understand the full scope of how these administrative hurdles impact your organization, you must look at the mastering multi-state Medicaid provider enrollment process, which is often even more rigorous and prone to delays than commercial insurance. Escaping Purgatory: Proactive Management as a Revenue Strategy The Veracity Group sees this play out every day. The difference between a practice that thrives and one that struggles with cash flow is often their approach to the provider enrollment landscape. You cannot afford to be reactive. Waiting for a denial to realize there is a problem means you are already
Telehealth Credentialing Across State Lines: Navigating the Midwest vs. West Medicaid Maze
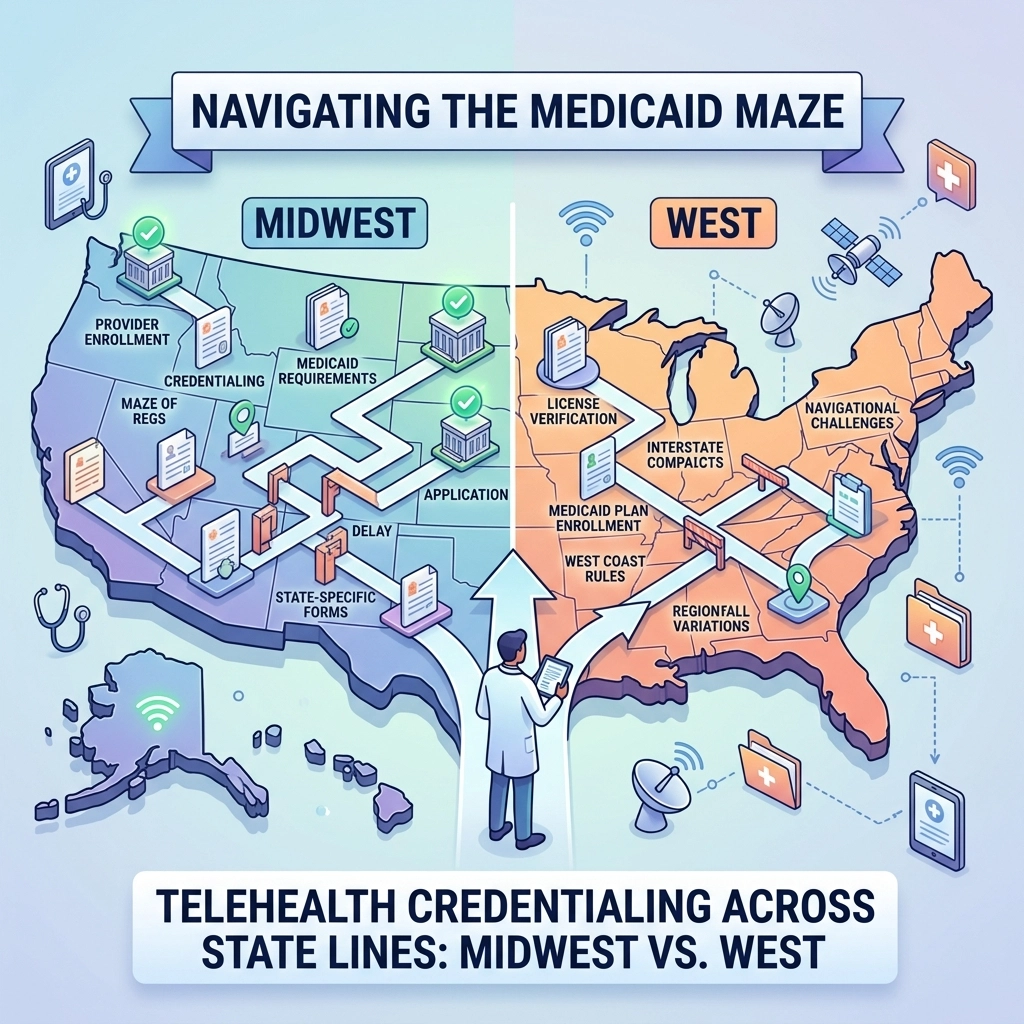
Navigating medical provider enrollment services across state lines while building a reliable telehealth footprint feels like playing a high-stakes game of 5D chess. Your patients do not care about state borders. They care about access to care from their living rooms. But the moment those pixels cross a state line, you enter a regulatory minefield. If you think a single license is your "golden ticket" to a national telehealth model, you are in for a rude awakening. Medicaid programs in Indiana, Illinois, and Nevada are not just different; they are entirely different ecosystems with unique "gotchas" that will stall your revenue if you are not prepared. If your question is "Can I see Medicaid patients across state lines?" the answer is simple: yes, but only after you satisfy each state's licensing, enrollment, and verification rules. If your question is "How do I do it without delays?" the answer is even clearer: you need a state-by-state process that matches your provider type, service location, and payer requirements. Looking for professional provider credentialing services in the USA? 👉 Check our main service page here: veracityeg.com The Golden Rule of the Virtual Visit Before we dive into the regional trenches, let’s establish the foundational law of the land: The provider must be licensed in the state where the patient is physically located at the time of the encounter. This is non-negotiable. Whether you are treating a patient via a smartphone in a cornfield in Indiana or a high-rise in Las Vegas, your legal right to practice is dictated by the ground under the patient’s feet. Failing to secure the correct state-specific enrollment is the fastest way to trigger a claim denial or, worse, an OIG audit. While the Interstate Medical Licensure Compact (IMLC) offers a streamlined pathway for physicians, the Medicaid enrollment process remains a manual, state-by-state slog that requires precision and insider knowledge. Alt-tag: A map of the United States highlighting the Midwest and Western regions for telehealth expansion. 1. The Midwest vs. the West: Streamlining vs. Complexity For general provider enrollment services, the Indiana-Illinois-Nevada comparison tells you exactly what multi-state expansion looks like in practice. One state removes friction. One state slows you down with administrative precision. One state raises the verification bar for every applicant. If you are asking where enrollment is easiest, where it gets sticky, and where extra documentation is non-negotiable, this three-state comparison is the focal point. Indiana: The License-Only Advantage If you have not looked at Indiana lately, you are missing a rare win for administrative efficiency. As of July 1, 2024, Indiana officially removed the requirement for telehealth-specific certificates. That creates a cleaner path for physicians, advanced practice providers, therapists, and other eligible clinicians expanding telehealth services under Medicaid. This is the key Indiana takeaway: if you hold the proper Indiana license, you do not need a separate telehealth certificate to move forward. That is a real operational advantage for multi-state groups asking, "Can I enroll in Indiana without another telehealth approval layer?" The answer is yes, provided your license, ownership information, service location details, and enrollment file are complete. However, do not mistake "easier" for "automatic." You still must submit accurate provider data to the Indiana Health Coverage Programs (IHCP). A clean Indiana rule set does not forgive sloppy applications. Illinois: The Administrative Precision State Cross the border into Illinois, and the vibe shifts. Illinois is the state that forces you to respect process discipline. The core question here is not whether telehealth is possible. The real question is how cleanly your enrollment file matches across every data source. For most medical specialties, Illinois becomes difficult for three reasons: Application detail must align across systems. Provider records must match state and payer files exactly. Delays compound quickly when ownership, practice location, or rendering-provider data is inconsistent. Illinois Medicaid is notoriously meticulous. If your CAQH profile is not synchronized perfectly with your state application, your file will sit in "pending" purgatory for months. That problem is not specialty-specific. It affects primary care, specialty care, surgical groups, therapy practices, and multi-location organizations alike. 2. The West: The Land of Stringent Verification If the Midwest is characterized by shifting legislative sands, the West: specifically Nevada: is characterized by its rigorous verification walls. While Western states often have strong telehealth infrastructure, their "gatekeeper" mentality for Medicaid is significantly more intense than what you will find in the heartland. Nevada: The "Gotcha" State Nevada does not play games. If you are looking to expand your footprint here, prepare for a verification marathon. Nevada Medicaid requires more stringent primary source verification and provider qualification documentation than Indiana or Illinois for many enrollment scenarios. This is the big Nevada question: "Can I enroll as an out-of-state provider if I already bill Medicaid elsewhere?" Yes, but Nevada will still require its own documentation trail, validation standards, and closer review. That is the "gotcha" many groups miss. Prior enrollment success in another state does not buy you a shortcut in Nevada. Nevada is particularly focused on out-of-state telehealth providers. The state wants to confirm that you are not operating as a "ghost clinic" and that every provider meets Nevada-specific requirements for licensure, qualifications, service locations, and supporting records. For general medical provider enrollment services, that means your file must be audit-ready before submission, not cleaned up after the fact. Alt-tag: A comparison chart showing the different requirements for Medicaid enrollment in Indiana, Illinois, and Nevada. Comparing the "Gotchas" Feature Indiana Illinois Nevada Telehealth Certificate Removed (as of 7/1/2024); license-only path is the key advantage Not the main issue; administrative alignment is the real hurdle Stricter review depends on provider type and enrollment facts Verification Speed Moderate Slow and detail-heavy Very stringent and documentation-heavy Key "Gotcha" Valid state license is enough for the telehealth approval piece, but the enrollment file still must be complete Data mismatches stall applications fast High scrutiny on out-of-state providers and stronger primary source verification Enrollment Difficulty Lower Medium-High High 3. Can You Enroll in Multiple Medicaid States at

