How to Credential a Sleep Medicine Provider: A Clinical Guide to Payer Enrollment

The landscape of Sleep Medicine is a complex intersection of multi-disciplinary expertise and rigorous facility standards. For practice managers and healthcare executives, the process of bringing a new sleep specialist into a network is not a routine administrative task; it is a high-stakes clinical and financial necessity. When you fail to navigate the specific nuances […]
How to Credential an Allergy Provider: Navigating Immunology and Payer Panels

The process of bringing a new specialist into your practice is the backbone of professional credibility and the primary driver of your revenue cycle. When you are looking at how to credential an allergy provider, the stakes are higher than in general medicine. Allergy and Immunology is a high-precision subspecialty that involves complex biologic therapies, […]
How to Credential an Addiction Medicine Provider: A Specialist’s Guide to Payer Enrollment

The demand for specialized addiction treatment has never been higher, yet the administrative hurdles to get these providers in-network remain some of the most complex in the healthcare industry. When you are looking at how to credential an addiction medicine provider, you aren’t just filling out standard forms; you are navigating a specialized landscape of […]
How to Credential a Dental Provider: A 2026 Guide to Specialty Enrollment
In the high-stakes landscape of 2026 healthcare, dental enrollment is no longer a administrative “back-burner” task: it is the backbone of your practice’s financial viability. For dental groups and solo practitioners alike, the ability to collect on claims hinges entirely on the precision of your specialty enrollment data. As commercial payers like Aetna and UnitedHealthcare […]
Payer Power Plays: Aetna, UHC & The 2026 Audit Surge

The landscape of healthcare reimbursement has officially shifted from passive oversight to aggressive litigation and algorithmic enforcement. As we move through March 2026, the industry is reeling from a series of high-stakes legal settlements and technological crackdowns that signal a new era of payer scrutiny. For clinic administrators and Revenue Cycle Management (RCM) leaders, the […]
Weekend Update: The 15-Day Rule & New State Laws You Can’t Ignore

March 2026 is delivering real, operationally relevant enrollment news—the kind that makes or breaks access and cash flow. If your providers are not enrolled and active, your practice does not get paid. Full stop. At The Veracity Group, we translate regulation into execution so you keep providers billable, audit-ready, and ready to scale across states […]
DEA, CSR, and State Licenses: The “Triple Threat” of Provider Onboarding

In the high-stakes environment of modern healthcare, the distance between hiring a top-tier provider and that provider actually seeing their first patient is often a bureaucratic chasm. This gap is defined by the "Triple Threat" of provider onboarding: State Medical Licensing, Controlled Substance Registration (CSR), and Federal DEA Registration. For healthcare administrators and practice owners, […]
Are Your Payer Contracts Costing You Money? (We Can Fix That)

For most medical practices, the primary focus is patient care. However, while you are focusing on clinical outcomes, your revenue is likely leaking through a sieve of outdated, unmonitored payer contracts. If you haven’t reviewed your payer agreements in the last twenty-four months, you are almost certainly leaving significant money on the table. The Veracity […]
5 DEA Registration Traps That Could Stop Your Practice

For any prescribing clinician, the Drug Enforcement Administration (DEA) registration is more than just a certificate on the wall; it is the fundamental authorization that allows you to treat patients effectively. Yet, despite its importance, the DEA registration system is notoriously rigid. It is built for regulatory compliance, not for user-friendliness. At The Veracity Group, […]
Provider Enrollment in New York: PNDS + Dual Eligible Unwind
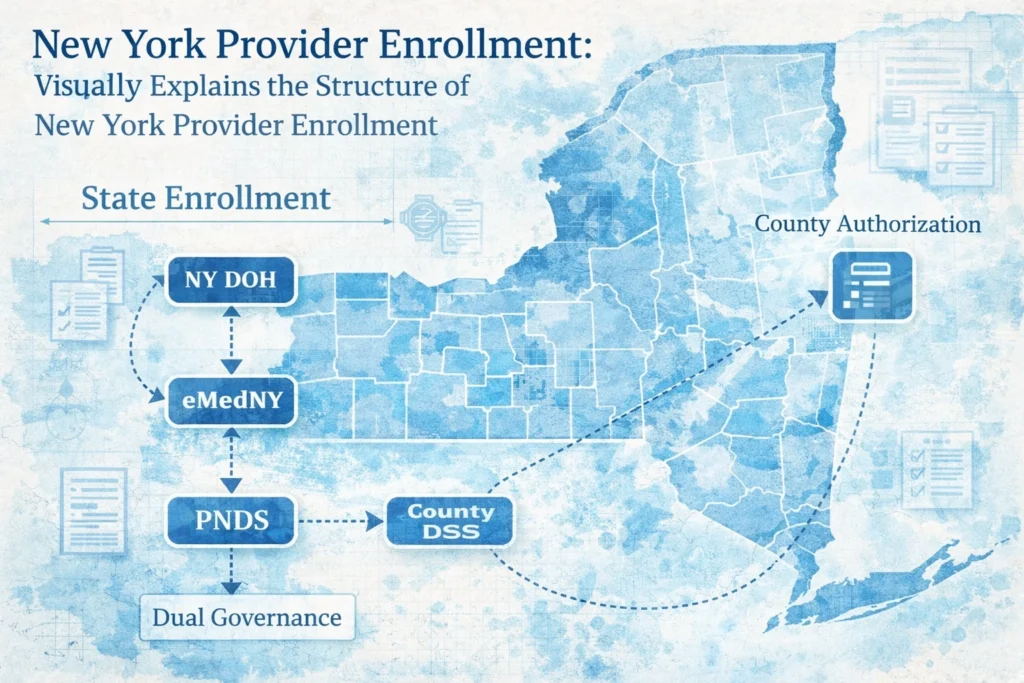
New York provider enrollment isn’t just complicated: it’s layered with administrative tripwires that derail even experienced practice managers. While most administrators focus on state-level Department of Health requirements, they miss how managed care network reporting, ongoing Provider Network Data System (PNDS) expectations, and NPI linking failures create a perfect storm of delays that cost your […]

